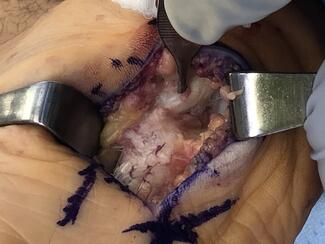
A Guide To Treating Common Rock Climbing Injuries In The Lower Extremity
Due to the advent of artificial rock climbing walls, the popularity of rock climbing has grown rapidly. In 2020, rock climbing will be featured for the first time as an Olympic sport. With this rapid increase in popularity comes an increase in the incidence of rock climbing-related injuries. Rock climbing injuries can be acute or chronic, and can involve both the upper and lower extremities. The majority of climbing-related injuries are overuse injuries of the upper extremity.1,2 Out of the acute injuries, however, nearly 50 percent involve the lower leg, ankle and foot.2-4
Acute lower extremity injuries can result from ground falls as well as arrested falls with trauma sustained from rock hit. This can include vertical forces from hitting ledges as well as horizontal forces from swinging in toward the rock wall. In contrast to acute injuries, rock climbers are often required to move on very small holds and the application of force over these very small areas results in high pressures where the foot contacts a hold. Additionally, climbing-specific shoe gear places significant forces on the foot. These high loads on the joints of the foot have the potential to cause chronic foot and ankle injuries.
Differentiating The Types Of Rock Climbing
There are several different styles of rock climbing that providers should understand in order to better assess injury risk.
• Bouldering involves climbing on smaller rock formations without the use of a harness and rope. Bouldering is typically limited in height to a safe fall distance and the only safety equipment people use is a ground pad or mat. Despite the use of these pads, bouldering does put the feet and ankles at increased risk of injury due to repetitive falling and potential falling from significant height.
• Free soloing is the most dangerous form of rock climbing as these climbers do not use protective gear and ascend climbing routes to heights where a fall would result in serious injury or death.
• Sport climbing and traditional climbing both use protective gear. Sport climbing relies on pre-placed protective bolts in the rock while traditional climbing requires the climber to place removable protective gear as he or she climbs. Traditional climbing can place climbers at higher fall risk due to the unpredictability of removable protective gear. Despite the use of protective gear, climbers have the potential to sustain lower extremity trauma from both ground fall (i.e. accidents with inadequate protection) or rock hit when the climber may hit ledges or swing back into the rock surface.
Understanding The Characteristics Of Rock Climbing Shoes
Rock climbing shoes are most often made of leather uppers with rubber toe and heel caps. The rubber of climbing shoes is specially formulated to stick to rock features and improve friction. Depending on individual preference as well as climbing difficulty level, these athletes may wear climbing shoes that are snug to extremely tight. Athletes who utilize climbing shoes often wear them several sizes smaller than street shoe size.
Among average ability climbers, Killian and colleagues found an average shoe size difference of one to two sizes between normal shoes and climbing shoes.5 Schoffl and Kupper reported that 87 percent of climbers noted a willingness to wear painful climbing shoes for better performance.4 Climbing shoes have variable features to improve performance on different terrain. These features include downturned toes for overhanging rock and stiff toe boxes for climbing shoes specific for crack climbing. While designed for performance, rock climbing shoes can contribute to many acute and chronic climbing-related injuries.
Addressing Toenail Injuries
Toenail injury. Toenail injuries are common in rock climbers. Subungual hematomas and distal tuft fractures can occur secondary to traumatic contact of the hallux, which usually occurs with swinging into the rock wall. Simon and Wolgin found distal phalanx fractures were associated with 37 percent of subungual hematomas, and more commonly occurred in hematomas involving 50 percent or more of the nail bed.6 Given this, radiographs are indicated when a subungual hematoma involves 50 percent or more of the nail bed, or when there is a high index of suspicion for associated fracture. Drainage by trephination or nail avulsion is generally indicated for subungual hematomas that are painful, less than 48 hours old and not spontaneously draining whereas smaller lesions may just need monitoring.
When it comes to distal tuft fractures, one should emphasize immobilization in a rigid-soled shoe. While distal phalanx fractures with associated subungual hematomas are open fractures, the routine use of prophylactic antibiotics in healthy individuals is not indicated. Seaberg and team found no infections in patients undergoing trephination and drainage of subungual hematoma without prophylactic antibiotic use, regardless of the size of hematoma or the presence of distal phalanx fracture.7
The literature is mixed regarding nail avulsion and bed repair with some studies favoring nail plate avulsion and repair of nail bed laceration while others show limited benefit.6,8 Repetitive nail trauma can lead to dystrophic nail changes and secondary fungal nail infection. Largiader and Oelz reported dystrophic nail changes in 28 percent of rock climbers while Buda and colleagues later found nail disease in 65.3 percent of climbers.9,10
Diagnosing And Treating Hallux Interphalangeal Joint And First MPJ Injuries
Hallux interphalangeal joint injury. Hallux interphalangeal joint disorders commonly occur in rock climbers. Valgus alignment of the hallux interphalangeal joint, exostosis, degenerative joint disease and bursa presence at the medial aspect of the joint can all lead to pain secondary to both tight shoe gear fit and the very narrow toe box of rock climbing shoes.
Treatment of hallux interphalangeal joint disorders can vary depending on the degree of severity. One can treat mild to moderate symptoms with offloading, ice, anti-inflammatory medications and corticosteroid injections. For more severe cases of hallux interphalangeal joint pathology, surgeons can perform surgical debridement, exostectomy, osteotomy or possible hallux interphalangeal joint fusion if there are associated degenerative joint changes.
First metatarsophalangeal joint injury. Both acute and chronic first MPJ injuries are common in rock climbers. Acute first MPJ injuries result from jamming insults, such as forcefully swinging into a wall or from forced dorsiflexion injuries occurring in ledge hit or ground fall. Milder acute injury of the great toe joint can occur with maximum load while pushing off footholds that isolate the great toe.
Clinicians can manage turf toe or hyperdorsiflexion injuries in the acute phase with rest, ice, non-steroidal anti-inflammatory drugs (NSAIDs) or immobilization, depending on injury severity.11 While surgical intervention is not frequently required, one may consider it if conservative treatment fails. Surgery of acute injuries most frequently involves excision of fractured sesamoid fragments or repair/reattachment of the first MPJ plantar plate.12
Repetitive axial loading can lead to chronic injury of the first MPJ and gradual degenerative joint changes. Additionally, shoe forces can cause biomechanical alterations of the foot such as foot shortening by supination, contracture of the lesser digits and valgus position of the hallux.5
Continued use of rock climbing shoes can contribute to the development of hallux valgus.13 There is an increased incidence of hallux valgus and hallux limitus among rock climbers. The general incidence of hallux valgus in adult males is 4.5 percent but Killian and colleagues report it to occur in 34 percent of average rock climbers and 53 percent of elite rock climbers.5
Researchers have noted an increasing frequency of hallux rigidus among rock climbers who require surgical intervention in the form of cheilectomy and fusion.14 Conservative management of hallux rigidus and hallux valgus in rock climbers includes splinting and limitation of first MPJ range of motion, accommodation of the deformity, anti-inflammatory medication and corticosteroid injection. Failure of conservative treatment warrants surgical intervention. In considering surgical options, providers should consider the loads placed on the first MPJ during climbing and avoid procedures such as aggressive arthroplasty, which may not provide adequate great toe joint stability for rock climbing, or implant arthroplasty, which may not be able to withstand the loads introduced during rock climbing.
Pertinent Insights On Treating Lisfranc Injuries
Lisfranc injury. Lisfranc joint injuries are the second most common foot injuries in athletes.15 While these injuries are most commonly reported in football and soccer, rock climbers are at high risk for these injuries as well. Mechanisms leading to Lisfranc injury can be low-energy or high-energy, and include indirect rotational force and axial load through a hyperplantarflexed forefoot.16-18 Resulting midfoot injuries can range from mild ligament sprain to severe fracture and dislocation. Due to minimal displacement or diastasis, these injuries can be difficult to diagnose and are often missed.19 Missed diagnosis of Lisfranc injury has the potential to increase risk of posttraumatic arthritis of the tarsometatarsal joints.
Management of Lisfranc injury varies depending on severity. Several classification systems exist for Lisfranc injuries with the majority focused on high-energy injuries.20,21 Nunley and Vertullo introduced a classification system for more subtle Lisfranc injuries.22 Given the high potential for morbidity with these injuries, conservative treatment is recommended only for functionally stable injuries.17,22,23 Operative treatment options for Lisfranc injuries include percutaneous reduction and internal fixation, open reduction and internal fixation, and primary arthrodesis, which is reserved for severe cases.17,22,23
When There Are Traumatic Hindfoot And Ankle Injuries
Hindfoot and ankle trauma. Ground fall injuries can result in a variety of lower extremity trauma. Small falls can result in contusions and injury to the plantar soft tissues.24 A fall from significant height can result in calcaneus, talus and ankle fractures depending on the lower extremity position at the time of impact.4,25 Hindfoot sprains, ankle sprains and soft tissue injury are also common rock climbing-related injuries. One study found that ankle injuries account for 19.2 percent of all climbing-related injuries.24 Gerdes and colleagues found ankles to be the site of 23 percent of sprain-type injuries and 22.1 percent of fractures while the foot accounted for 24.6 percent of climbing-related fractures.26
Standard podiatric principles apply for the management of hindfoot and ankle fractures with the majority of displaced, unstable and/or intra-articular fractures undergoing open reduction and internal fixation. For minor soft tissue injuries, clinicians can manage these patients with rest, ice and immobilization while more significant injuries may require primary surgical repair. Soft tissue injuries that fail initial conservative management may require subsequent surgical repair.
How To Handle Bouldering-Specific Injuries
Bouldering-specific injury. Bouldering frequently relies on mats or pads to cushion falls. The use of these mats has led to a unique injury mechanism with ankle injuries sustained when the foot lands on the outermost edge of the pad or lands between two pads.4 These injuries can lead to ankle fracture and ligamentous injury with the potential for subsequent ankle instability.
One should manage all displaced ankle fractures operatively in appropriate surgical candidates. Ligamentous injuries may respond to immobilization and physical therapy. Physicians can address cases of chronic instability surgically with many modalities including primary repair/imbrication, local tendon transfer, tendon autograft or allograft stabilization procedures.
Recognizing Contributing Factors With Chronic Rock-Climbing Injuries
Chronic rock climbing-related injuries. The majority of rock climbing-related literature has focused on acute foot and ankle injuries. Studies examining chronic rock-climbing injuries are mostly limited to the upper extremity. Buda and colleagues did perform one study examining overuse injuries among rock climbers.10 This study found foot and/or ankle pathology in 86 percent of the 144 rock climbers surveyed.10 Injuries included nail disease (65.3 percent), ankle instability (27.8 percent), retrocalcaneal bursitis (19.4 percent), Achilles tendinitis (12.5 percent), metatarsalgia (12.5 percent) and plantar fasciitis (5.6 percent). Factors associated with overuse injury included male sex, higher degree of rock climbing difficulty, higher rock climbing shoe heel counter, competitive climbing level and rock climbing shoes 2.3 sizes smaller than common footwear.10
In Conclusion
With its increasing popularity and growing access to climbing gyms, rock climbing injuries are becoming more commonplace. In order to provide accurate diagnosis and subsequent treatment, providers should be familiar with the mechanisms that can result in foot and ankle injuries among rock climbers. Knowledge of the high mechanical loads athletes encounter when climbing is important when treating related injuries. Moving forward, further research is necessary to better understand optimal treatment protocols for rock climbing-related injuries.
Dr. Hoffman is an Attending Physician in the Department of Orthopedics at Denver Health Medical Center. She is an Assistant Professor in the Department of Orthopedics at the University of Colorado School of Medicine. She is an Attending Physician for the Highland/Presbyterian St. Luke’s Medical Center Residency Program.
Dr. Thompson is an Assistant Professor of Exercise Science at Fort Lewis College in Durango, Colo. She specializes in biomechanics, neuroscience and human gait.
1. Jones G, Asghar A, Llewellyn DJ. The epidemiology of rock-climbing injuries. Br J Sports Med. 2008;42(9):773-778.
2. Backe S, Ericson L, Janson S, Timpka T. Rock climbing injury rates and associated risk factors in a general climbing population. Scand J Med Sci Sports. 2009;19(6):850-856.
3. Schoffl V, Morrison A, Schoffl I, Kupper T. The epidemiology of injury in mountaineering, rock and ice climbing. Med Sport Sci. 2012;58:17-43.
4. Schoffl V, Kupper T. Feet injuries in rock climbers. World J Orthop. 2013;4(4):218-228.
5. Killian RB, Nishimoto GS, Page JC. Foot and ankle injuries related to rock climbing. The role of footwear. J Am Podiatr Med Assoc. 1998;88(8):365- 374.
6. Simon RR, Wolgin M. Subungual hematoma: association with occult laceration requiring repair. Am J Emerg Med. 1987;5(4):302-304.
7. Seaberg DC, Angelos WJ, Paris PM. Treatment of subungual hematomas with nail trephination: a prospective study. Am J Emerg Med. 1991;9(3):209-210.
8. Roser SE, Gellman H. Comparison of nail bed repair versus nail trephination for subungual hematomas in children. J Hand Surg Am. 1999;24(6):1166-1170.
9. Largiader U, Oelz O. An analysis of overstrain injuries in rock climbing. Schweiz Z. Sportmed. 1993;41(3):107-114.
10. Buda R, Di Caprio F, Bedetti L, Mosca M, Giannini S. Foot overuse diseases in rock climbing: an epidemiologic study. J Am Podiatr Med Assoc. 2013;103(2):113-120.
11. McCormick JJ, Anderson RB. Turf toe: anatomy, diagnosis, and treatment. Sports Health. 2010;2(6):487-494.
12. Covell DJ, Lareau CR, Anderson RB. Operative treatment of traumatic hallux valgus in elite athletes. Foot Ankle Int. 2017;38(6):590-595.
13. van der Putten EP, Snijder CJ. Shoe design for prevention of injuries in sport climbing. Appl Ergon. 2001;32(4):379-387.
14. Hochholzer T, Schoeffl V. One Move Too Many. 2nd ed. Lochner-Verlag: Ebenhausen, Germany; 2006.
15. Meyer SA, Callaghan JJ, Albright JP, Crowley ET, Powell JW. Midfoot sprains in collegiate football players. Am J Sports Med. 1994;22(3):392-401.
16. Vuori JP, Aro HT. Lisfranc joint injuries: trauma mechanisms and associated injuries. J Trauma. 1993;35(1):40-45.
17. Desmond EA, Chou LB. Current concepts review: Lisfranc injuries. Foot Ankle Int. 2006;27(8):653-660.
18. Shapiro MS, Wascher DC, Finerman GA. Rupture of Lisfranc’s ligament in athletes. Am J Sports Med. 1994;22(5):687-691.
19. Burroughs KE, Reimer CD, Fields KB. Lisfranc injury of the foot: a commonly missed diagnosis. Am Fam Phys. 1998;58(1):118-124.
20. Quenu E KG. Etude sur les luxutations du metatarse (luxations metatarso-tarsiennes) du diastasis entre le 1. et le 2. metatarsien. Rev Chir Paris. 1909;39:281–336.
21. Myerson MS, Fisher RT, Burgess AR, Kenzora JE. Fracture dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle. 1986;6(5):225-242.
22. Nunley JA, Vertullo CJ. Classification, investigation, and management of midfoot sprains: Lisfranc injuries in the athlete. Am J Sports Med. 2002;30(6):871-878.
23. Watson TS, Shurnas PS, Denker J. Treatment of Lisfranc joint injury: current concepts. J Am Acad Orthop Surg. 2010;18(12):718-728.
24. Neuhof A, Hennig FF, Schoffl I, Schoffl V. Injury risk evaluation in sport climbing. Int J Sports Med. 2011;32(10):794-800.
25. Blanchette MA, Grenier JM. Fracture of the lateral tubercle of the posterior talar process caused by a rock-climbing fall: a case report. J Can Chiropr Assoc. 2014;58(3):286-290.
26. Gerdes EM, Hafner JW, Aldag JC. Injury patterns and safety practices of rock climbers. J Trauma. 2006;61(6):1517-1525.