Third-Degree Burns Due to Copper Compression Sock: Concerns for Patients With Neuropathy
A recent case report involving a 68-year-old patient with type 2 diabetes and peripheral neuropathy examines how wearing a copper-containing compression sock while sitting in the sun for several hours led to third-degree burns. The patient was treated with sharp debridement, dressing management, and tubular compression and was healing well before being lost to follow-up. The report highlights the need for healthcare providers and medical device sellers to educate wearers about potential risks in using these compression garments
For many patients with peripheral neuropathy, compression socks provide relief from a range of conditions. Studies of compression garments show clear benefits and few complications, with most being minor, but this case brings light to the need for further research into the possibility of copper- and silver-containing compression socks leading to injury through heat transfer, particularly among wearers with neuropathy. In fact, the author of this study notes “a well-documented history of patients with neuropathy developing thermal burns from heat sources.”
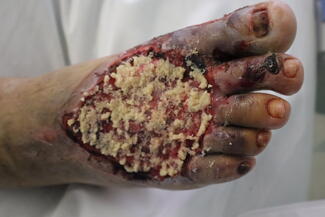
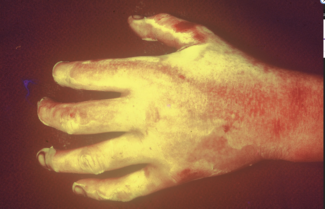
This case report follows a 68-year-old man with a left below-knee amputation and history of type 2 diabetes, in addition to several other comorbidities. While wearing a compression sock containing copper, the patient reported spending 3 hours sitting in the sun on May 1, 2020. He noted that his leg later “felt funny,” and removal of the compression sock revealed blistering on the skin of his lower right leg.
The patient’s initial care began 2 days later with a telehealth appointment with an urgent care physician due to the COVID-19 pandemic. Silvadene dressings and a 10-day course of prophylactic clindamycin were prescribed, along with a recommendation to follow up in person within 1-2 days. At an in-person evaluation the following day, the patient’s physician reported partial-thickness burns to the shin and foot and noted neuropathy that started about one-third of the way down the patient’s lower right leg.
On June 2, the patient requested a referral to the wound clinic, where he was seen 10 days later. The physical evaluation at that time revealed 6 open wounds which, based on photos taken by the patient on May 2, were identified as third-degree burns surrounded by areas of second-degree burns. Treatment at the wound clinic included sharp debridement and application of honey gel to remaining necrotic areas as well as silver foam to areas with granulation tissue. Tubular compression was applied, and the patient received instruction on performing daily dressing changes. He was also educated about the significance of blood glucose control for healing. The wounds showed excellent healing 5 weeks later, after which the patient was lost to follow-up.
In response to this incident, the report’s author informed the seller of the patient’s compression socks of this adverse event, and a report was filed with the FDA Safety Information and Adverse Event Reporting Program. The author writes, “Patients with diabetes, and especially patients with diabetes and neuropathy, are at risk of developing more severe burns as well as complications following thermal injury, which makes it paramount that they receive education about burn prevention. Such education should be specific regarding possible sources of burns. Future research is recommended to examine the thermal conductivity of metal-containing clothing.”
Reference: Gallentine A. Third-Degree Burn on the Neuropathic Lower Extremity in a Patient With Diabetes While Wearing a Copper–Containing Compression Sock: A Case Report. Index Wound Manag Prev. 2021;67(11):26–29