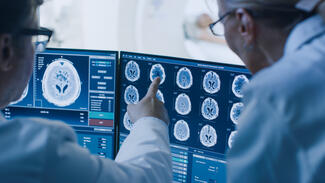
Key Benefits and Indications for Non-Invasive Home Mechanical Ventilation
“Home mechanical ventilation has really advanced, and I don't think many of us realize that,” says Jaspal Singh, MD, MHA, MHS, Pulmonary Oncology and Critical Care Education medical director at Atrium Health Levine Cancer Institute, Charlotte, North Carolina.
In this video, Dr Singh reviews the evolving role of noninvasive home mechanical ventilation beyond traditional continuous positive airway pressure therapy in sleep disorder care. He discusses indications across chronic respiratory and neurologic conditions, highlights benefits such as reduced work of breathing, and emphasizes individualized, physiology-driven device selection alongside practical considerations in the United States care setting.
For more expert insights, visit the Sleep Disorders Excellence Forum here on Pulmonology Learning Network.
Key Clinical Takeaways
- Home noninvasive ventilation (NIV), including continuous positive airway pressure (CPAP), bilevel positive airway pressure (BiPAP), and advanced devices, provides respiratory support for patients with chronic obstructive pulmonary disease (COPD), emphysema, amyotrophic lateral sclerosis (ALS), and spinal cord injury by improving ventilation, reducing breathing effort, and supporting nighttime respiratory function.
- Device selection requires a clinically driven assessment of patient physiology, including oxygen and carbon dioxide abnormalities, respiratory strength, disease progression, and the need for interfaces, alarms, secretion clearance, and adjunct therapies to avoid adverse sequelae.
- In the United States Medicare setting, bilevel positive airway pressure (BiPAP) devices may transition to patient ownership within approximately one year, whereas advanced devices may result in ongoing rental costs, making appropriate device selection critical for both clinical and financial outcomes.
Read the Transcript
Jaspal Singh, MD, MHA, MHS: Hi everybody. I'm Dr Jaspal Singh. I'm in Charlotte, North Carolina. I'm a pulmonary critical care and sleep physician. I practice in a large medical center and an outpatient clinic where we manage a host of patients with pulmonary sleep and critical care disorders.
Pulmonology Learning Network (PLN): Can you provide a brief overview of the different types of non-invasive home mechanical ventilation?
Dr Singh: Home mechanical ventilation has really advanced. I don't think many of us realize. I think back when I trained, a lot of us might've trained in a day where we told sort of things just CPAP therapy. And CPAP therapy, what looks like a local CPAP device now, could be one of many things that can provide pretty sophisticated positive airway pressure therapy options at home.
When we talk about home non-invasive ventilation, generally speaking, that usually means beyond traditional CPAP therapy. But for some people actually, it can be positive airway pressure therapy from a CPAP, BiPAP, all the way to more sophisticated advancements, such as how much pressure. You can drive the pressure very high. You can do volume control, you can do pressure modality modes, you can do where the machine has a backup rates that are pretty sophisticated in their algorithm. But the idea is that basically home mechanical ventilation provides respiratory support at home. How you do that and the way it's done actually is clearly evolving. At least from my lens from as a pulmonologist and a sleep physician and even critical care, I sometimes see that a lot of clinicians don't really understand how critical the right device can be for that person short-term and long-term. That device selection and that initial experience can have a lot of sequelae if not done appropriately well.
PLN: What are the key indications and benefits of non-invasive home mechanical ventilation?
Dr Singh: Well, non-invasive mechanical ventilation has several key benefits. It depends really on what it's being used for. So, a classic indication might be someone has trouble breathing at home, has a chronic lung disease, for example, take COPD and emphysema, and they're just having a hard time when they go home to really maneuver to get enough air movement at night. Or they spend so much effort breathing that actually that fatigues them, that tires them out, and they're not able to do their usual things. So oftentimes we use non-invasive mechanical ventilation at the home for chronic respiratory illnesses. That may be respiratory, it could be neurological, for example, a spinal cord injury or a disease like amyotrophic lateral sclerosis, ALS. So those diseases oftentimes require respiratory support delivered through a nasal or mouth interface or both that allows air to be entered and with lot less effort.
PLN: Using shared decision-making, how does a care team determine which HMV is best for a patient?
Dr Singh: How does a care team decide which one is set? I'd like to think it's nuanced based on clinical aspects, and that I think a high-performing team would do that. Some of my colleagues around the country are just experts at this. They just know this patient's physiology, let's understand it, let's understand how strong their lungs are, how strong their respiratory drive is, whether is it an oxygen problem or a carbon dioxide problem or both, and to what degree? I think a nuanced approach that understands the patient's disease processes, their physiology, and deciding what type of machine they need and what type of interface that machine has. Also, what type of alarms that person needs. Do they need alarm systems at home in case something happens? Do they need adjuncts like things to help the patient cough, to clear secretions? Do they need some medicines in addition to augment some of the other positive area pressure delivery?
I think all those things are very nuanced. I like to think it's all clinically driven, but sometimes there are pragmatic aspects to it. For example, a lot of places, depending on your comfort with managing the home mechanical ventilation, there might be just not the expertise available. There might be payment mechanisms that make people go to one choice or the other. And that can be very challenging for our patients who are trying to just get through this really difficult clinical situation and they probably don't understand the implications of those decisions. Let me be specific. If somebody, for example, only needs a bi-level device, for example, BiPAP therapy, as might be called, with maybe a backup rate, that's a fairly simple device relatively speaking to get a patient for, and what's nice about at least in the US, if they're on Medicare and they actually are moving towards owning that device within a year. If for some reason someone says, "You know what, that patient's very sick, they need a more advanced device, and they get them on a more advanced device, even though patient may not need it, then there's actually financial potential implications because that patient may be paying rent on that device or fees on that device for eternity."
So, people are looking at this at a national level, trying to understand the nuances here, the implications here, but at least for now, I think at the very least, try to understand what your patient needs today. And if they can get by with a less complicated device that might beneficial for them. On the same token, if they have a progressive disease that's relentless, like a neuromuscular disorder, you want to get them the right device soon that will hopefully be able to last for some time and fulfill their patient's physiological needs as their disease evolves.
Jaspal Singh, MD, MHA, MHS, is board-certified in internal medicine, pulmonary disease, sleep medicine, and critical care medicine. He specializes in treating lung nodules, lung cancer, pleural effusions, obstructive sleep apnea and mechanical ventilation. He is the medical director for Innovation and Quality Improvement for Pulmonary Oncology at Atrium Health Levine Cancer Institute and the medical director for Critical Care Practice and Education at the Jan & Ed Brown Center for Pulmonary Medicine. He received his medical degree at the University of Illinois. He completed residency at the University of Rochester (Strong Memorial Hospital), and fellowship training at Duke University Medical Center.
© 2024 HMP Global. All Rights Reserved.
Any views and opinions expressed above are those of the author(s) and do not necessarily reflect the views, policy, or position of the Pulmonology Learning Network or HMP Global, their employees, and affiliates.