HS Immunopathogenesis Drives Expansion of Targeted Therapeutic Strategies
Hidradenitis suppurativa (HS) represents one of the most immunologically complex inflammatory skin diseases, with emerging insights into its pathogenesis reshaping the therapeutic landscape, according to James Krueger, MD, PhD, during his Music City SCALE 2026 presentation, “Current Perspective on Hidradenitis Suppurativa and Treatment Landscape.”
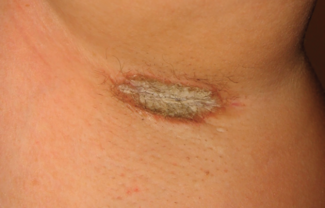
HS is characterized clinically by inflammatory nodules, abscesses, and purulent drainage from dermal tunnels, often accompanied by progressive tissue destruction and scarring. Dr Krueger emphasized that the disease is marked by “high systemic inflammation” and a variable, progressive course, underscoring the need for early recognition and intervention.
At the tissue level, HS involves disruption of key epithelial structures. Early disease is defined by nodules and abscesses, while advanced disease includes epithelialized tunnels and sinus tracts within the deep dermis. These structures serve as conduits for inflammatory activity, contributing to chronic drainage and tissue damage. Histologically, there is widespread leukocyte infiltration throughout the dermis, with neutrophil-rich purulent discharge representing a hallmark of late-stage disease.
Beyond innate immune activation, the presentation highlighted a significant role for adaptive immunity. B cells and plasma cells are abundant within HS lesions, with evidence of increased immunoglobulin production. Dr Krueger noted that “polyclonal IgGs are among the highest up-regulated mRNAs in HS lesions,” reflecting a robust humoral immune response. The chemokine CXCL13, which recruits B cells, is also highly expressed, further supporting this pathway.
These findings have therapeutic implications. Bruton’s tyrosine kinase, a key regulator of B-cell signaling, was identified as a “viable target in HS,” suggesting a potential shift toward therapies that address both innate and adaptive immune mechanisms.
The evolving treatment landscape reflects this complexity. Current investigational strategies include targeting IL-17A and IL-17F, TNF and OX40L pathways, and multiple IL-1 family cytokines. Additional approaches include JAK1 inhibition for patients with TNF inhibitor failure and bispecific antibodies that simultaneously target multiple inflammatory pathways.
Novel modalities, such as nanobody-based therapies and molecular traps, are also under investigation, aiming to enhance specificity and tissue penetration.
For more meeting coverage, visit the Music City SCALE newsroom.
Reference
Krueger J. Current perspective on hidradenitis suppurativa and treatment landscape. Presented at: Music City SCALE Symposium; May 13–17, 2026; Nashville, TN.