The year 2013 has brought many exciting advances in the field of dermatology, particularly in the realm of biologic drugs and in melanoma treatment. In fact, there were so many discoveries that this year in review just touches on some of the highlights of the past year. Areas within the field of dermatology with recent significant advances include infectious disease, acne/rosacea, biologics, psoriasis, cutaneous malignancies, contact dermatitis, atopic dermatitis, pediatric dermatology, cosmetic dermatology and HLA allele associations.
Infectious Disease
MRSA Decolonization in Intensive Care Units
Huang et al found that washing every patient in intensive care units (ICUs) daily with chlorhexidine-impregnated cloths and 5 days of twice-daily intranasal mupirocin treatments reduced positive cultures of methicillin-resistant Staphylococcus aureus (MRSA) by 37% and reduced bloodstream infection from any pathogen by 44%.1 The study included 74,256 patients and 74 ICUs. Hospitals were divided into 3 groups: group 1, implemented MRSA screening and isolation; group 2, targeted decolonization (ie, screening, isolation and decolonization of MRSA carriers) and group 3, universal decolonization (ie, no screening and decolonization of all patients). Universal decolonization was more effective than targeted decolonization or screening and isolation in reducing rates of MRSA clinical isolates and bloodstream infection from any pathogen. This implies that our current standard of isolating patients with MRSA is less effective than previously believed.
New Antibiotics for the Treatment of Skin Infections
Tedizolid phosphate (Cubist Pharmaceuticals/Trius Therapeutics) may be a reasonable alternative to linezolid for treating acute bacterial skin and skin structure infections (ABSSSI), which includes cellulitis or erysipelas, major cutaneous abscesses and wound infections. ESTABLISH-1, a Phase III trial, found that 6-day oral tedizolid phosphate (200 mg once daily) was as effective as 10 days of oral linezolid (600 mg every 12 hours) for treatment of ABSSSI.2 Outcomes included early response, measured 48-72 hours after initiating therapy, and sustained clinical responses at the end of treatment (day 11) and at the post-therapy evaluation visit (7-14 days after the end of treatment); both early and sustained responses of tedizolid were non-inferior to linezolid. This shorter dosing period of tedizolid may also improve patient adherence.
The Medicines Company has developed oritavancin, a lipoglycopeptide with a long half-life and rapid bactericidal activity againstgram-positive bacteria, including MRSA. In fact, 1 single, 1200 mg intravenous (IV) dose of oritavancin was found to be as effective as a 7- to 10-day dose of vancomycin for acute bacterial and structural skin infections.3 At 48-72 hours there was cessation of spread or reduction in size of the baseline lesion, the absence of fever and no requirement for rescue antibiotics (82.3% for oritavancin vs 78.9% for vancomycin). MRSA infections had similar outcomes (80.8% for oritavancin vs 80.0% for vancomycin). Rates of adverse events were similar in the 2 groups; 60.0% of the oritavancin group reported at least 1 adverse event, as did 63.8% of the vancomycin group. If implemented, this antibiotic could substantially reduce hospital admissions for IV antibiotics.
New Topical Treatments for Tinea Pedis and Onychomycosis
The topical allylamine naftifine hydrochloride 2% gel (Merz North America) was found to be well-tolerated and effective in treating both interdigital-type and moccasin-type tinea pedis in a large, randomized, controlled trial.4 After only 2 weeks of daily application, patients treated with naftifine gel 2% demonstrated statistically significant improvement from baseline in terms of complete cure, mycological cure and treatment effectiveness. Improvements continued with time; at 6 weeks the treatment group achieved 22% complete cure, 62% mycologic cure and 52% treatment effectiveness (P< 0.0001 for all 3 categories). In July, Naftin (naftifine HCl) Gel 2%, (Merz North America) received FDA approval, for the treatment of interdigital tinea pedis caused by the organisms Trichophyton rubrum, T. mentagrophytes and Epidermophyton floccosum in patients 18 years of age and older.
Another topical antifungal agent, luliconazole cream 1% (Luzu, Topica Pharmaceuticals), an imidazole, was found in a double-blind, vehicle-controlled study to be safe and effective for treatment at 2 week or 4 weeks for interdigital tinea pedis.5 At 2 weeks, 26.8% of the treatment group achieved complete clearance, and at 4 weeks 45.7% achieved complete clearance (compared to controls 9.1% and 10.0%, respectively). More importantly, the antifungal effects of luliconazole persisted for several weeks, resulting in increased rates of mycological cure. Luliconazole cream 1% received FDA approval in November for the topical treatment of interdigital tinea pedis, tinea cruris and tinea corporis, caused by the organisms T. rubrum and E. floccosum, in patients 18 years of age and older.
Prior to this year, topical treatments for onychomycosis were only modestly effective. However, a novel topical triazole antifungal, efinaconazole (Valeant Pharmaceuticals International, Inc) was shown in Phase II and Phase III studies to be effective in treating mild-to-moderate toenail distal lateral subungual onychomycosis (DLSO).6,7 In Phase II studies, mycologic cure rates with efinaconazole 10% semiocclusion, efinaconazole 10% and efinaconazole 5% were 83%, 87% and 87%, respectively.6 At follow-up, complete cure was also higher in the treatment groups, ranging from 16%-26%. This study provided evidence that once-daily efinaconazole 10% solution applied topically for 36 weeks was more effective than vehicle in treating DLSO.
In these 2 Phase III studies, the treatment arm received 48 weeks of efinaconazole 10% solution, and were evaluated at week 52.7 Mycologic cure rates were significantly greater with efinaconazole, ranging from roughly 53%-55%. Complete cure in these studies ranged from 15%-18%. This is exciting news for patients and dermatologists alike, as the side-effect profile is much safer than oral medications.
Efficacy of Antimycobacterial Treatment in Sarcoidosis
The possibility for mycobacterial contribution in the pathogenesis of sarcoidosis prompted this Phase I, randomized, placebo-controlled trial of 30 patients with chronic cutaneous sarcoidosis.8 The trial investigated the role of concomitant levofloxacin, ethambutol, azithromycin and rifampin (CLEAR) therapy. Results showed the CLEAR group had statistically decreased lesion size and granuloma burden with 8 weeks of treatment compared to placebo. In the intention-to-treat analysis, the CLEAR-treated group experienced a decrease in mean index lesion size from 22.4 mm to 14.0 mm (P=0.008), whereas the 15 patients assigned to placebo experienced a non-significant increase in mean index lesion size from 17.1 mm to 17.9 mm (P=0.05 for the difference between groups).
Acne/Rosacea
New Treatment for Pre-Adolescent Acne
 On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
Brimonidine FDA Approved for Erythema Associated with Rosacea
On August 26, 2013, the FDA approved brimonidine topical gel 0.33% (Mirvaso, Galderma Laboratories) as the first and only topical treatment specifically indicated for the persistent facial erythema resulting from rosacea. It is a highly selective alpha-2 adrenergic receptor agonist and acts via vasoconstriction to improve erythema associated with rosacea. It is applied once daily to adults age 18 and older, and results last up to 12 hours.
 In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
Biologics
Omalizumab for Chronic Idiopathic or Spontaneous Urticaria
Genentech and Novartis Pharmaceuticals’ omalizumab (Xolair) was found to significantly reduce disease severity in patients with a chronic idiopathic urticaria who failed standard therapy. This Phase III, multi-center, randomized, double-blind study evaluated patients with moderate-to-severe chronic idiopathic urticaria who were still symptomatic while taking H-antihistamine therapy.11
After 12 weeks of treatment with omalizumab, the itch-severity score was significantly decreased in a dose-dependent relationship. Omalizumab, when administered as 3 doses of 150 mg or 300 mg at 4-week intervals, significantly reduced the weekly itch-severity score as compared with placebo; 150 mg of omalizumab (–8.1±6.4; P=0.001) and 300 mg of omalizumab (–9.8±6.0; P<0.001). Serious adverse events were rare, most of them occurring in the 300-mg group where they occurred in 6% of patients.
Adalimumab for Sarcoidosis
Adalimumab (Humira, AbbVie Inc) was effective in treating cutaneous sarcoidosis in a double-blind, randomized, placebo-controlled trial.12 After 12 weeks, there was improvement specifically in target lesion area in the adalimumab-treated patients relative to placebo recipients (P=.0203). At the end of the additional 12-week, open-label phase, there was significant improvement in target lesion area (P=.0063), target lesion volume (P=.0225) and Dermatology Life Quality Index score (P=.0034). While adalimumab was effective for cutaneous disease, it had no effect on pulmonary function tests, radiographic findings or laboratory studies.
Psoriasis
 Novel Janus Kinase Inhibitor Improves Psoriasis
Novel Janus Kinase Inhibitor Improves Psoriasis
Oral treatments are now being developed for psoriasis. Tofacitinib (Xeljanz, Pfizer Inc), a novel, oral Janus kinase inhibitor, has been shown to objectively and subjectively improve psoriasis. Results from Phase IIb trials found Psoriasis Area and Severity Index (PASI) 75 response rates were higher for all twice-daily doses: 25%, (2 mg), 41% (5 mg) and 67% (15 mg) compared to placebo (2%) at 12 weeks.13 Results from the Phase IIb, 12-week trial showed that tofacitinib also improved patient-reported outcomes.14 The study included patients with moderate-to-severe chronic plaque psoriasis who were candidates for systemic therapy or phototherapy. Treatment with tofacitinib 2 mg, 5 mg and 15 mg twice daily resulted in generally dose-dependent improvements in several patient-reported outcomes measures compared with placebo.
Secukinumab in Moderate-to-Severe Plaque Psoriasis
Novartis Pharmaceuticals’ secukin-umab, a fully human IgG1κ monoclonal anti-interleukin-17A antibody, was shown to significantly improve psoriasis in recent Phase II trials. After 12 weeks of treatment, 83% of patients randomized to receive 3 time monthly 150 mg doses achieved a PASI 75.15 In addition, 52% of the patients in this dosing regimen achieved a PASI 90 at 12 weeks. Secukinumab was well-tolerated, although 2 cases of neutropenia were reported in the treatment arm.
Ustekinumab for Psoriatic Arthritis
On September 23, 2013, ustekinumab (Stelara, Janssen Biotech Inc) alone or in combination with methotrexate was FDA approved for the treatment of psoriatic arthritis in patients age 18 and older. The fully human monoclonal antibody improved active psoriatic arthritis, despite treatment with disease-modifying anti-rheumatic drugs and/or non-steroidal anti-inflammatory drugs, in a Phase III trial (PSUMMIT 1).16 In the 45-mg group, 42.4% of patients saw a 20% improvement in their symptoms according to the criteria of the American College of Rheumatology (ACR20) at week 24. In the 90-mg group, 49.5% of patients achieved ACR20. In addition, ACR responses were greater with ustekinumab than placebo regardless of methotrexate use. Treatment was generally well-tolerated with similar proportions of patients in the treatment and placebo group experiencing adverse events at week 16.
Drug Therapy Improves Patient-Related Outcomes for Psoriatic Arthritis
A Phase IIb trial revealed that apremilast (Celgene Corporation), a specific inhibitor of phosphodiesterase 4, was successful at treating psoriatic arthritis as measured by several patient-related outcomes.17 Apremilast 20 mg twice a day resulted in statistically significant and clinically meaningful improvements in health-related quality of life, pain and global visual analog scale and Functional Assessment of Chronic Illness Therapy-Fatigue scores.
Cutaneous Malignancies
Donor Contribution to the Malignant Skin Epithelium in Kidney Transplantation
It is well-known that patients who receive organ transplants are at increased risk for squamous cell carcinoma. However, a new study found that it is possible that the actual donor may also contribute to this increased risk.18 In 21 skin squamous cell carcinomas from kidney transplant recipients, the researchers examined p53 expression TP53 mutations. In 1 patient, skin tumor cells that were the same genotype as the donated kidney also contained the same TP53 mutation. This may provide evidence for a donor contribution to the malignant skin epithelium in allogeneic kidney transplantation.
Risk Factors for Poor Outcome in Squamous Cell Carcinomas
In a new, single-center, 10-year retrospective, cohort study, 5 risk factors were identified that were associated with recurrence and death from cutaneous squamous cell carcinomas. The 5 major factors were: (1) tumor diameter of at least 2 cm; (2) invasion beyond fat; (3) poor cellular differentiation; (4) perineural invasion and (5) ear, temple or anogenital location.19 The researchers evaluated 985 patients who had a total of 1,832 tumors. The median follow-up was 50 months.
Melanoma Prognosis in Young Men
 A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
Imatinib for KIT-Mutatnt Melanomas
Imatinib (Gleevec, Novartis Pharmaceuticals) has shown efficacy in patients with KIT-mutant melanoma in a multi-center, Phase II trial.21 Of the patients with KIT mutations or amplification in melanomas arising from acral, mucosal or chronically sun-damaged sites, the response rate was 21%. KIT mutations should be analyzed in these locations, because imatinib now represents a viable treatment option.
Combination Therapy for Melanoma
In a Phase I trial, treatment of advanced melanoma with concurrent therapy of ipilimumab (Yervoy, Bristol-Myers Squibb) with the experimental nivolumab (Bristol-Myers Squibb) was very promising.22 The study examined both concurrent therapy and sequential therapy, and found the former to be superior. Furthermore, the objective response rates of concurrent therapy also exceeded the previously reported results of nivolumab and ipilimumab monotherapy. The superior response with combination therapy is thought to be secondary to targeting different immune checkpoints: ipilimumab is an antibody against cytotoxic T-lymphocyte-associated antigen 4, and nivolumab is an antibody against the programmed death 1 receptor. The objective response rate with the concurrent use of the 2 therapies was 40% (N=53 patients). Furthermore, in those patients receiving a maximum dose (associated with an acceptable level of adverse events), ipilimumab (3 mg/kg/day) and nivolumab (1 mg/kg/day), the objective response rate was 53%, all with tumor reduction of 80% or more. Adverse events were common with Grade 3 or Grade 4 therapy- related adverse events in 53% of patients in the concurrent regimen; however, these were manageable and were generally reversible. The most common side effects included elevated levels of lipase (13%), aspartate aminotransferase (13%) and alanine aminotransferase (11%).
A Phase II trial for metastatic melanoma also showed benefit with combination therapy; in this instance, ipilimumab was combined with a granulocyte-macrophage colony-stimulating factor, sargramostim (Leukine, sanofi-aventis).23 Combining therapy in this case not only prolonged survival, but caused fewer serious side effects and deaths compared with ipilimumab alone. The median overall survival for the combination was 17.5 months, while ipilimumab monotherapy was 12.7 months (P=.0014). There was also a 35% decrease in risk of dying with combination therapy than those treated with ipilimumab alone.
Contact Dermatitis
Methylisothiazolinone Is the Allergen of the Year
The American Contact Dermatitis Society named the preservative/biocide methylisothiazolinone (MI) as the 2013 Allergen of the Year.24 Methylisothiazolinone is found in face creams, mascaras, shampoos, body washes and wet wipes, and is increasingly being used in the United States. Patch testing with the methylchloroisothiazolinone/MI mix misses approximately 40% of those allergic to MI, most likely secondary to the low MI concentration in the mix. It is has been recommended that routine screening of MI take place with patch testing series.
Atopic Dermatology
Allergic Contact Dermatitis in Patients with Atopic Dermatitis
 Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Pediatric Dermatology
Recommendations for the Use of Propranolol in Infantile Hemangiomas
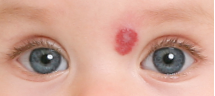 Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Recommendations included when to treat complicated IH; contraindications and pre-treatment evaluation protocols; propranolol use in PHACE syndrome; formulation, target dose and frequency of propranolol; initiation of propranolol in infants; cardiovascular monitoring; ongoing monitoring and prevention of hypoglycemia. It was universally agreed that an electrocardiogram should be part of the pre-treatment evaluation in instances where patients had below normal heart rate, or if patients have a family history of arrhythmias or maternal history of connective tissue disease. The recommended initial dosing for propranolol was 1 mg/kg/day (at a concentration of 20 mg/5 mL) divided into 3 times daily and than titrated up to a target dose. It was also recommended that propranolol be discontinued during illness to prevent hypoglycemia. Furthermore, recommendations regarding ongoing monitoring and PHACE syndrome screening and treatment are outlined within the guidelines. These new guidelines are valuable to the medical community given the frequency that IH occur and the prior lack of recommendations.
Timolol for Hemangiomas
Timolol has been studied in non-randomized trials, but a recent randomized, controlled trial evaluated timolol maleate 0.5% gel on superficial focal hemangiomas in a 24-week study of infants age 5 to 24 weeks.27
The results showed timolol applied twice a day significantly reduced proportional growth and lesion volume compared to placebo. The efficacy of timolol was more pronounced for lesions with a mean diameter of <11.3 mm (<100 mm3). In addition, clinical appearance improved; the blinded photo evaluation at 24 weeks found that 47% of actively treated lesions were free of redness compared to only 6% of lesions in the placebo group. Patients treated with timolol gel began to show efficacy at 12 weeks to 16 weeks, much later than the effect seen after starting oral propranolol, which usually is noticeable at 48 hours. However, based on the study results, timolol appears safe with no significant differences in heart rate or systolic or diastolic blood pressures.
Cosmetic Dermatology
Picosecond 755-nm Alexandrite Laser for Tattoo Removal
 A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
OnabotulinumtoxinA FDA approved for Lateral Canthal Lines
 On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
HLA Allele Associations
HLA-B*1502 Allele Association with SJS and TEN in Patients Using Carbamazepine
A new meta-analysis showed a significant association between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) within specific races. Han-Chinese, Thais, Koreans and Malaysians have approximately 115-fold, 60-fold, 25-fold and 220-fold increased risk of developing SJS or TEN with this HLA allele, respectively.30 The FDA currently recommends HLA-B*1502 allele before initiation of carbamazepine therapy in Asian patients. Despite these recommendations, there was still some debate about the relationship between HLA-B*1502 and SJS and TEN among patients taking carbamazepine, especially within some races. These findings provide an overwhelming relationship between the HLA-B*1502 allele and carbamazepine-induced SJS and TEN within specific races, the implications of which will hopefully lead to more standardized genetic testing before initiation of carbamazepine therapy.
Summary
It has been another exciting year in dermatology. We appreciate all the dedicated clinicians and researchers that have contributed to this year’s dermatology advances, from oral medication for psoriasis to new treatment options for melanoma. We look forward to all scientific and therapeutic advances on the horizon for 2014 and beyond. n
Dr. De Luca is with the department of dermatology at Wake Forest University School of Medicine in Winston-Salem, NC.
Disclosure: Dr. De Luca has no conflicts of interest to report.
References
1. Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368(24):2255-2265.
2. Prokocimer P, De Anda C, Fang E, Mehra P, Das A. Tedizolid phosphate vs linezolid for treatment of acute bacterial skin and skin structure infections: the ESTABLISH-1 randomized trial. JAMA. 2013;309(6):559-569.
3. Corey R, Perez A, Moeck G, et al. A single-dose of oritavancin (ORI) is comparable to 7-10 days of vancomycin (VAN) in the treatment of acute bacterial skin and skin structure infections (ABSSSI): the SOLO I study. Presented at: 53rd Interscience Conference on Antimicrobial Agents and Chemotherapy; September 10, 2013; Denver, CO. Abstract L-204.
4. Stein Gold LF, Parish LC, Vlahovic T, et al. Efficacy and safety of naftifine HCl Gel 2% in the treatment of interdigital and Moccasin type tinea pedis: pooled results from two multicenter, randomized, double-blind, vehicle-controlled trials.
J Drugs Dermatol. 2013;12(8):911-918.
5. Jarratt M, Jones T, Kempers S, et al. Luliconazole for the treatment of interdigital tinea pedis: A double-blind, vehicle-controlled study. Cutis. 2013;91(4):203-210.
6. Tschen EH, Bucko AD, Oizumi N, Kawabata H, Olin JT, Pillai R. Efinaconazole solution in the treatment of toenail onychomycosis: a phase 2, multicenter, randomized, double-blind study.
J Drugs Dermatol. 2013;12(2):186-192.
7. Elewski BE, Rich P, Pollak R, et al. Efinaconazole 10% solution in the treatment of toenail onychomycosis: Two phase III multicenter, randomized, double-blind studies. J Am Acad Dermatol. 2013;68(4):600-608.
8. Drkae WF, Oswald-Richter K, Richmond BW, et al. Oral antimycobacterial therapy in chronic cutaneous sarcoidosis: a randomized, single-masked, placebo-controlled study. JAMA Dermatol. 2013;149(9):1040-1049.
9. Eichenfield LF, Draelos Z, Lucky AW, et al. Preadolescent moderate acne vulgaris: a randomized trial of the efficacy and safety of topical adapalene-benzoyl peroxides. J Drugs Dermatol. 2013;12(6):611-618.
10. Fowler J Jr, Jackson M, Moore A, et al. Efficacy and safety of once-daily topical brimonidine tartrate gel 0.5% for the treatment of moderate to severe facial erythema of rosacea: results of two randomized, double-blind, and vehicle-controlled pivotal studies. Drugs Dermatol. 2013;12(6):650-656.
11. Maurer M, Rosén K, Hsieh HJ, et al. Omalizumab for the treatment of chronic idiopathic or spontaneous urticaria. N Engl J Med. 2013;368(10):924-935.
12. Pariser RJ, Paul J, Hirano S, Torosky C, Smith M. A double-blind, randomized, placebo-controlled trial of adalimumab in the treatment of cutaneous sarcoidosis. J Am Acad Dermatol. 2013;68(5):765-773.
13. Papp KA, Menter A, Strober B, et al. Efficacy and safety of tofacitinib, an oral Janus kinase inhibitor, in the treatment of psoriasis: a Phase 2b randomized placebo-controlled dose-ranging study. Br J Dermatol. 2012;167(3):668-677.
14. Mamolo C, Harness J, Tan H, Menter A. Tofacitinib (CP-690,550), an oral Janus kinase inhibitor, improves patient-reported outcomes in a phase 2b, randomized, double-blind, placebo-controlled study in patients with moderate-to-severe psoriasis. J Eur Acad Dermatol Venereol. Published online ahead of print January 7, 2013.
15. Papp KA, Langley RG, Sigurgeirsson B, et al. Efficacy and safety of secukinumab in the treatment of moderate-to-severe plaque psoriasis: a randomized, double-blind, placebo-controlled phase II dose-ranging study. Br J Dermatol. 2013;168(2):412-421.
16. McInnes IB, Kavanaugh A, Gottlieb AB, et al. Efficacy and safety of ustekinumab in patients with active psoriatic arthritis: 1 year results of the phase 3, multicentre, double-blind, placebo-controlled PSUMMIT 1 trial. Lancet, 2013;382(9894):780-789.
17. Strand V, Schett G, Stevens RM. Patient-reported Health-related Quality of Life with apremilast for psoriatic arthritis: a phase II, randomized, controlled study. J Rheumatol. 2013;40(7):1158-1165.
18. Verneuil L, Varna M, Ratajczak P, et al. Human skin carcinoma arising from kidney transplant-derived tumor cells. J Clin Invest. 2013;123(9):3797-801.
19. Schmults CD, Karia PS, Carter JB, Han J, Qureshi AA. Factors predictive of recurrence and death from cutaneous squamous cell carcinoma: a 10-year, single-institution cohort study. JAMA Dermatol. 2013;149(5):541-547.
20. Gamba CS, Clarke CA, Keegan TH, Tao L, Swetter SM. Melanoma survival disadvantage in young, non-Hispanic white males compared with females. JAMA Dermatol. 2013;149(8):912-920.
21. Hodi FS, Corless CL, Giobbie-Hurder A, et al. Imatinib for melanomas harboring mutationally activated or amplified KIT arising on mucosal, acral, and chronically sun-damaged skin. J Clin Oncol. 2013;31(26):3182-3190.
22. Wolchok JD, Kluger H, Callahan MK, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369(2):122-133.
23. American Association for Cancer Research. GM-CSF/Ipilimumab combination extends melanoma survival. Cancer Discov. 2013;3(7):OF6.
24. Castanedo-Tardana MP, Zug KA. Methylisothiazolinone. Dermatitis. 2013;24(1):2-6.
25. Malajian D, Belsito DV. Cutaneous delayed-type hypersensitivity in patients with atopic dermatitis. J Am Acad Dermatol. 2013;69(2):232-237.
26. Drolet BA, Frommelt PC, Chamlin SL, et al. Initiation and use of propranolol for infantile hemangioma: report of a consensus conference. Pediatrics. 2013;131(1):128-140.
27. Chan H, McKay C, Adams S, Wargon O. RCT of timolol maleate gel for superficial infantile hemangiomas in 5- to 24-week-olds. Pediatrics. 2013;131(6):e1739-e1747.
28. Saedi N, Metelitsa A, Patrell K, Arndt KA, Dover JS. Treatment of tattoos with a picosecond alexandrite laser: a prospective trial. Arch Dermatol. 2012;148(12):1360-1363.
29. FDA approves Botox Cosmetic to improve appearance of crow’s feet lines. FDA website. https://www.fda.gov/newsevents/newsroom/pressannouncements/ucm367662.htm. Accessed November 13, 2013.
30. Tangamornsuksan W, Chaiyakunapruk N, Somkrua R, Lohitnavy M, Tassaneeyakul W. Relationship between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson Syndrome and toxic epidermal necrolysis: a systematic review and meta-analysis. JAMA Dermatol. 2013;149(9):1025-1032.
The year 2013 has brought many exciting advances in the field of dermatology, particularly in the realm of biologic drugs and in melanoma treatment. In fact, there were so many discoveries that this year in review just touches on some of the highlights of the past year. Areas within the field of dermatology with recent significant advances include infectious disease, acne/rosacea, biologics, psoriasis, cutaneous malignancies, contact dermatitis, atopic dermatitis, pediatric dermatology, cosmetic dermatology and HLA allele associations.
Infectious Disease

MRSA Decolonization in Intensive Care Units
Huang et al found that washing every patient in intensive care units (ICUs) daily with chlorhexidine-impregnated cloths and 5 days of twice-daily intranasal mupirocin treatments reduced positive cultures of methicillin-resistant Staphylococcus aureus (MRSA) by 37% and reduced bloodstream infection from any pathogen by 44%.1 The study included 74,256 patients and 74 ICUs. Hospitals were divided into 3 groups: group 1, implemented MRSA screening and isolation; group 2, targeted decolonization (ie, screening, isolation and decolonization of MRSA carriers) and group 3, universal decolonization (ie, no screening and decolonization of all patients). Universal decolonization was more effective than targeted decolonization or screening and isolation in reducing rates of MRSA clinical isolates and bloodstream infection from any pathogen. This implies that our current standard of isolating patients with MRSA is less effective than previously believed.
New Antibiotics for the Treatment of Skin Infections
Tedizolid phosphate (Cubist Pharmaceuticals/Trius Therapeutics) may be a reasonable alternative to linezolid for treating acute bacterial skin and skin structure infections (ABSSSI), which includes cellulitis or erysipelas, major cutaneous abscesses and wound infections. ESTABLISH-1, a Phase III trial, found that 6-day oral tedizolid phosphate (200 mg once daily) was as effective as 10 days of oral linezolid (600 mg every 12 hours) for treatment of ABSSSI.2 Outcomes included early response, measured 48-72 hours after initiating therapy, and sustained clinical responses at the end of treatment (day 11) and at the post-therapy evaluation visit (7-14 days after the end of treatment); both early and sustained responses of tedizolid were non-inferior to linezolid. This shorter dosing period of tedizolid may also improve patient adherence.
The Medicines Company has developed oritavancin, a lipoglycopeptide with a long half-life and rapid bactericidal activity againstgram-positive bacteria, including MRSA. In fact, 1 single, 1200 mg intravenous (IV) dose of oritavancin was found to be as effective as a 7- to 10-day dose of vancomycin for acute bacterial and structural skin infections.3 At 48-72 hours there was cessation of spread or reduction in size of the baseline lesion, the absence of fever and no requirement for rescue antibiotics (82.3% for oritavancin vs 78.9% for vancomycin). MRSA infections had similar outcomes (80.8% for oritavancin vs 80.0% for vancomycin). Rates of adverse events were similar in the 2 groups; 60.0% of the oritavancin group reported at least 1 adverse event, as did 63.8% of the vancomycin group. If implemented, this antibiotic could substantially reduce hospital admissions for IV antibiotics.

New Topical Treatments for Tinea Pedis and Onychomycosis
The topical allylamine naftifine hydrochloride 2% gel (Merz North America) was found to be well-tolerated and effective in treating both interdigital-type and moccasin-type tinea pedis in a large, randomized, controlled trial.4 After only 2 weeks of daily application, patients treated with naftifine gel 2% demonstrated statistically significant improvement from baseline in terms of complete cure, mycological cure and treatment effectiveness. Improvements continued with time; at 6 weeks the treatment group achieved 22% complete cure, 62% mycologic cure and 52% treatment effectiveness (P< 0.0001 for all 3 categories). In July, Naftin (naftifine HCl) Gel 2%, (Merz North America) received FDA approval, for the treatment of interdigital tinea pedis caused by the organisms Trichophyton rubrum, T. mentagrophytes and Epidermophyton floccosum in patients 18 years of age and older.
Another topical antifungal agent, luliconazole cream 1% (Luzu, Topica Pharmaceuticals), an imidazole, was found in a double-blind, vehicle-controlled study to be safe and effective for treatment at 2 week or 4 weeks for interdigital tinea pedis.5 At 2 weeks, 26.8% of the treatment group achieved complete clearance, and at 4 weeks 45.7% achieved complete clearance (compared to controls 9.1% and 10.0%, respectively). More importantly, the antifungal effects of luliconazole persisted for several weeks, resulting in increased rates of mycological cure. Luliconazole cream 1% received FDA approval in November for the topical treatment of interdigital tinea pedis, tinea cruris and tinea corporis, caused by the organisms T. rubrum and E. floccosum, in patients 18 years of age and older.
Prior to this year, topical treatments for onychomycosis were only modestly effective. However, a novel topical triazole antifungal, efinaconazole (Valeant Pharmaceuticals International, Inc) was shown in Phase II and Phase III studies to be effective in treating mild-to-moderate toenail distal lateral subungual onychomycosis (DLSO).6,7 In Phase II studies, mycologic cure rates with efinaconazole 10% semiocclusion, efinaconazole 10% and efinaconazole 5% were 83%, 87% and 87%, respectively.6 At follow-up, complete cure was also higher in the treatment groups, ranging from 16%-26%. This study provided evidence that once-daily efinaconazole 10% solution applied topically for 36 weeks was more effective than vehicle in treating DLSO.
In these 2 Phase III studies, the treatment arm received 48 weeks of efinaconazole 10% solution, and were evaluated at week 52.7 Mycologic cure rates were significantly greater with efinaconazole, ranging from roughly 53%-55%. Complete cure in these studies ranged from 15%-18%. This is exciting news for patients and dermatologists alike, as the side-effect profile is much safer than oral medications.
Efficacy of Antimycobacterial Treatment in Sarcoidosis
The possibility for mycobacterial contribution in the pathogenesis of sarcoidosis prompted this Phase I, randomized, placebo-controlled trial of 30 patients with chronic cutaneous sarcoidosis.8 The trial investigated the role of concomitant levofloxacin, ethambutol, azithromycin and rifampin (CLEAR) therapy. Results showed the CLEAR group had statistically decreased lesion size and granuloma burden with 8 weeks of treatment compared to placebo. In the intention-to-treat analysis, the CLEAR-treated group experienced a decrease in mean index lesion size from 22.4 mm to 14.0 mm (P=0.008), whereas the 15 patients assigned to placebo experienced a non-significant increase in mean index lesion size from 17.1 mm to 17.9 mm (P=0.05 for the difference between groups).
Acne/Rosacea
New Treatment for Pre-Adolescent Acne
 On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
Brimonidine FDA Approved for Erythema Associated with Rosacea
On August 26, 2013, the FDA approved brimonidine topical gel 0.33% (Mirvaso, Galderma Laboratories) as the first and only topical treatment specifically indicated for the persistent facial erythema resulting from rosacea. It is a highly selective alpha-2 adrenergic receptor agonist and acts via vasoconstriction to improve erythema associated with rosacea. It is applied once daily to adults age 18 and older, and results last up to 12 hours.
 In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
Biologics
Omalizumab for Chronic Idiopathic or Spontaneous Urticaria
Genentech and Novartis Pharmaceuticals’ omalizumab (Xolair) was found to significantly reduce disease severity in patients with a chronic idiopathic urticaria who failed standard therapy. This Phase III, multi-center, randomized, double-blind study evaluated patients with moderate-to-severe chronic idiopathic urticaria who were still symptomatic while taking H-antihistamine therapy.11
After 12 weeks of treatment with omalizumab, the itch-severity score was significantly decreased in a dose-dependent relationship. Omalizumab, when administered as 3 doses of 150 mg or 300 mg at 4-week intervals, significantly reduced the weekly itch-severity score as compared with placebo; 150 mg of omalizumab (–8.1±6.4; P=0.001) and 300 mg of omalizumab (–9.8±6.0; P<0.001). Serious adverse events were rare, most of them occurring in the 300-mg group where they occurred in 6% of patients.
Adalimumab for Sarcoidosis
Adalimumab (Humira, AbbVie Inc) was effective in treating cutaneous sarcoidosis in a double-blind, randomized, placebo-controlled trial.12 After 12 weeks, there was improvement specifically in target lesion area in the adalimumab-treated patients relative to placebo recipients (P=.0203). At the end of the additional 12-week, open-label phase, there was significant improvement in target lesion area (P=.0063), target lesion volume (P=.0225) and Dermatology Life Quality Index score (P=.0034). While adalimumab was effective for cutaneous disease, it had no effect on pulmonary function tests, radiographic findings or laboratory studies.
Psoriasis
 Novel Janus Kinase Inhibitor Improves Psoriasis
Novel Janus Kinase Inhibitor Improves Psoriasis
Oral treatments are now being developed for psoriasis. Tofacitinib (Xeljanz, Pfizer Inc), a novel, oral Janus kinase inhibitor, has been shown to objectively and subjectively improve psoriasis. Results from Phase IIb trials found Psoriasis Area and Severity Index (PASI) 75 response rates were higher for all twice-daily doses: 25%, (2 mg), 41% (5 mg) and 67% (15 mg) compared to placebo (2%) at 12 weeks.13 Results from the Phase IIb, 12-week trial showed that tofacitinib also improved patient-reported outcomes.14 The study included patients with moderate-to-severe chronic plaque psoriasis who were candidates for systemic therapy or phototherapy. Treatment with tofacitinib 2 mg, 5 mg and 15 mg twice daily resulted in generally dose-dependent improvements in several patient-reported outcomes measures compared with placebo.
Secukinumab in Moderate-to-Severe Plaque Psoriasis
Novartis Pharmaceuticals’ secukin-umab, a fully human IgG1κ monoclonal anti-interleukin-17A antibody, was shown to significantly improve psoriasis in recent Phase II trials. After 12 weeks of treatment, 83% of patients randomized to receive 3 time monthly 150 mg doses achieved a PASI 75.15 In addition, 52% of the patients in this dosing regimen achieved a PASI 90 at 12 weeks. Secukinumab was well-tolerated, although 2 cases of neutropenia were reported in the treatment arm.
Ustekinumab for Psoriatic Arthritis
On September 23, 2013, ustekinumab (Stelara, Janssen Biotech Inc) alone or in combination with methotrexate was FDA approved for the treatment of psoriatic arthritis in patients age 18 and older. The fully human monoclonal antibody improved active psoriatic arthritis, despite treatment with disease-modifying anti-rheumatic drugs and/or non-steroidal anti-inflammatory drugs, in a Phase III trial (PSUMMIT 1).16 In the 45-mg group, 42.4% of patients saw a 20% improvement in their symptoms according to the criteria of the American College of Rheumatology (ACR20) at week 24. In the 90-mg group, 49.5% of patients achieved ACR20. In addition, ACR responses were greater with ustekinumab than placebo regardless of methotrexate use. Treatment was generally well-tolerated with similar proportions of patients in the treatment and placebo group experiencing adverse events at week 16.
Drug Therapy Improves Patient-Related Outcomes for Psoriatic Arthritis
A Phase IIb trial revealed that apremilast (Celgene Corporation), a specific inhibitor of phosphodiesterase 4, was successful at treating psoriatic arthritis as measured by several patient-related outcomes.17 Apremilast 20 mg twice a day resulted in statistically significant and clinically meaningful improvements in health-related quality of life, pain and global visual analog scale and Functional Assessment of Chronic Illness Therapy-Fatigue scores.
Cutaneous Malignancies

Donor Contribution to the Malignant Skin Epithelium in Kidney Transplantation
It is well-known that patients who receive organ transplants are at increased risk for squamous cell carcinoma. However, a new study found that it is possible that the actual donor may also contribute to this increased risk.18 In 21 skin squamous cell carcinomas from kidney transplant recipients, the researchers examined p53 expression TP53 mutations. In 1 patient, skin tumor cells that were the same genotype as the donated kidney also contained the same TP53 mutation. This may provide evidence for a donor contribution to the malignant skin epithelium in allogeneic kidney transplantation.
Risk Factors for Poor Outcome in Squamous Cell Carcinomas
In a new, single-center, 10-year retrospective, cohort study, 5 risk factors were identified that were associated with recurrence and death from cutaneous squamous cell carcinomas. The 5 major factors were: (1) tumor diameter of at least 2 cm; (2) invasion beyond fat; (3) poor cellular differentiation; (4) perineural invasion and (5) ear, temple or anogenital location.19 The researchers evaluated 985 patients who had a total of 1,832 tumors. The median follow-up was 50 months.
Melanoma Prognosis in Young Men
 A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
Imatinib for KIT-Mutatnt Melanomas
Imatinib (Gleevec, Novartis Pharmaceuticals) has shown efficacy in patients with KIT-mutant melanoma in a multi-center, Phase II trial.21 Of the patients with KIT mutations or amplification in melanomas arising from acral, mucosal or chronically sun-damaged sites, the response rate was 21%. KIT mutations should be analyzed in these locations, because imatinib now represents a viable treatment option.
Combination Therapy for Melanoma
In a Phase I trial, treatment of advanced melanoma with concurrent therapy of ipilimumab (Yervoy, Bristol-Myers Squibb) with the experimental nivolumab (Bristol-Myers Squibb) was very promising.22 The study examined both concurrent therapy and sequential therapy, and found the former to be superior. Furthermore, the objective response rates of concurrent therapy also exceeded the previously reported results of nivolumab and ipilimumab monotherapy. The superior response with combination therapy is thought to be secondary to targeting different immune checkpoints: ipilimumab is an antibody against cytotoxic T-lymphocyte-associated antigen 4, and nivolumab is an antibody against the programmed death 1 receptor. The objective response rate with the concurrent use of the 2 therapies was 40% (N=53 patients). Furthermore, in those patients receiving a maximum dose (associated with an acceptable level of adverse events), ipilimumab (3 mg/kg/day) and nivolumab (1 mg/kg/day), the objective response rate was 53%, all with tumor reduction of 80% or more. Adverse events were common with Grade 3 or Grade 4 therapy- related adverse events in 53% of patients in the concurrent regimen; however, these were manageable and were generally reversible. The most common side effects included elevated levels of lipase (13%), aspartate aminotransferase (13%) and alanine aminotransferase (11%).
A Phase II trial for metastatic melanoma also showed benefit with combination therapy; in this instance, ipilimumab was combined with a granulocyte-macrophage colony-stimulating factor, sargramostim (Leukine, sanofi-aventis).23 Combining therapy in this case not only prolonged survival, but caused fewer serious side effects and deaths compared with ipilimumab alone. The median overall survival for the combination was 17.5 months, while ipilimumab monotherapy was 12.7 months (P=.0014). There was also a 35% decrease in risk of dying with combination therapy than those treated with ipilimumab alone.
Contact Dermatitis
Methylisothiazolinone Is the Allergen of the Year
The American Contact Dermatitis Society named the preservative/biocide methylisothiazolinone (MI) as the 2013 Allergen of the Year.24 Methylisothiazolinone is found in face creams, mascaras, shampoos, body washes and wet wipes, and is increasingly being used in the United States. Patch testing with the methylchloroisothiazolinone/MI mix misses approximately 40% of those allergic to MI, most likely secondary to the low MI concentration in the mix. It is has been recommended that routine screening of MI take place with patch testing series.
Atopic Dermatology
Allergic Contact Dermatitis in Patients with Atopic Dermatitis
 Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Pediatric Dermatology
Recommendations for the Use of Propranolol in Infantile Hemangiomas
 Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Recommendations included when to treat complicated IH; contraindications and pre-treatment evaluation protocols; propranolol use in PHACE syndrome; formulation, target dose and frequency of propranolol; initiation of propranolol in infants; cardiovascular monitoring; ongoing monitoring and prevention of hypoglycemia. It was universally agreed that an electrocardiogram should be part of the pre-treatment evaluation in instances where patients had below normal heart rate, or if patients have a family history of arrhythmias or maternal history of connective tissue disease. The recommended initial dosing for propranolol was 1 mg/kg/day (at a concentration of 20 mg/5 mL) divided into 3 times daily and than titrated up to a target dose. It was also recommended that propranolol be discontinued during illness to prevent hypoglycemia. Furthermore, recommendations regarding ongoing monitoring and PHACE syndrome screening and treatment are outlined within the guidelines. These new guidelines are valuable to the medical community given the frequency that IH occur and the prior lack of recommendations.
Timolol for Hemangiomas
Timolol has been studied in non-randomized trials, but a recent randomized, controlled trial evaluated timolol maleate 0.5% gel on superficial focal hemangiomas in a 24-week study of infants age 5 to 24 weeks.27
The results showed timolol applied twice a day significantly reduced proportional growth and lesion volume compared to placebo. The efficacy of timolol was more pronounced for lesions with a mean diameter of <11.3 mm (<100 mm3). In addition, clinical appearance improved; the blinded photo evaluation at 24 weeks found that 47% of actively treated lesions were free of redness compared to only 6% of lesions in the placebo group. Patients treated with timolol gel began to show efficacy at 12 weeks to 16 weeks, much later than the effect seen after starting oral propranolol, which usually is noticeable at 48 hours. However, based on the study results, timolol appears safe with no significant differences in heart rate or systolic or diastolic blood pressures.
Cosmetic Dermatology
Picosecond 755-nm Alexandrite Laser for Tattoo Removal
 A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
OnabotulinumtoxinA FDA approved for Lateral Canthal Lines
 On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
HLA Allele Associations
HLA-B*1502 Allele Association with SJS and TEN in Patients Using Carbamazepine
A new meta-analysis showed a significant association between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) within specific races. Han-Chinese, Thais, Koreans and Malaysians have approximately 115-fold, 60-fold, 25-fold and 220-fold increased risk of developing SJS or TEN with this HLA allele, respectively.30 The FDA currently recommends HLA-B*1502 allele before initiation of carbamazepine therapy in Asian patients. Despite these recommendations, there was still some debate about the relationship between HLA-B*1502 and SJS and TEN among patients taking carbamazepine, especially within some races. These findings provide an overwhelming relationship between the HLA-B*1502 allele and carbamazepine-induced SJS and TEN within specific races, the implications of which will hopefully lead to more standardized genetic testing before initiation of carbamazepine therapy.
Summary
It has been another exciting year in dermatology. We appreciate all the dedicated clinicians and researchers that have contributed to this year’s dermatology advances, from oral medication for psoriasis to new treatment options for melanoma. We look forward to all scientific and therapeutic advances on the horizon for 2014 and beyond. n
Dr. De Luca is with the department of dermatology at Wake Forest University School of Medicine in Winston-Salem, NC.
Disclosure: Dr. De Luca has no conflicts of interest to report.
References
1. Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368(24):2255-2265.
2. Prokocimer P, De Anda C, Fang E, Mehra P, Das A. Tedizolid phosphate vs linezolid for treatment of acute bacterial skin and skin structure infections: the ESTABLISH-1 randomized trial. JAMA. 2013;309(6):559-569.
3. Corey R, Perez A, Moeck G, et al. A single-dose of oritavancin (ORI) is comparable to 7-10 days of vancomycin (VAN) in the treatment of acute bacterial skin and skin structure infections (ABSSSI): the SOLO I study. Presented at: 53rd Interscience Conference on Antimicrobial Agents and Chemotherapy; September 10, 2013; Denver, CO. Abstract L-204.
4. Stein Gold LF, Parish LC, Vlahovic T, et al. Efficacy and safety of naftifine HCl Gel 2% in the treatment of interdigital and Moccasin type tinea pedis: pooled results from two multicenter, randomized, double-blind, vehicle-controlled trials.
J Drugs Dermatol. 2013;12(8):911-918.
5. Jarratt M, Jones T, Kempers S, et al. Luliconazole for the treatment of interdigital tinea pedis: A double-blind, vehicle-controlled study. Cutis. 2013;91(4):203-210.
6. Tschen EH, Bucko AD, Oizumi N, Kawabata H, Olin JT, Pillai R. Efinaconazole solution in the treatment of toenail onychomycosis: a phase 2, multicenter, randomized, double-blind study.
J Drugs Dermatol. 2013;12(2):186-192.
7. Elewski BE, Rich P, Pollak R, et al. Efinaconazole 10% solution in the treatment of toenail onychomycosis: Two phase III multicenter, randomized, double-blind studies. J Am Acad Dermatol. 2013;68(4):600-608.
8. Drkae WF, Oswald-Richter K, Richmond BW, et al. Oral antimycobacterial therapy in chronic cutaneous sarcoidosis: a randomized, single-masked, placebo-controlled study. JAMA Dermatol. 2013;149(9):1040-1049.
9. Eichenfield LF, Draelos Z, Lucky AW, et al. Preadolescent moderate acne vulgaris: a randomized trial of the efficacy and safety of topical adapalene-benzoyl peroxides. J Drugs Dermatol. 2013;12(6):611-618.
10. Fowler J Jr, Jackson M, Moore A, et al. Efficacy and safety of once-daily topical brimonidine tartrate gel 0.5% for the treatment of moderate to severe facial erythema of rosacea: results of two randomized, double-blind, and vehicle-controlled pivotal studies. Drugs Dermatol. 2013;12(6):650-656.
11. Maurer M, Rosén K, Hsieh HJ, et al. Omalizumab for the treatment of chronic idiopathic or spontaneous urticaria. N Engl J Med. 2013;368(10):924-935.
12. Pariser RJ, Paul J, Hirano S, Torosky C, Smith M. A double-blind, randomized, placebo-controlled trial of adalimumab in the treatment of cutaneous sarcoidosis. J Am Acad Dermatol. 2013;68(5):765-773.
13. Papp KA, Menter A, Strober B, et al. Efficacy and safety of tofacitinib, an oral Janus kinase inhibitor, in the treatment of psoriasis: a Phase 2b randomized placebo-controlled dose-ranging study. Br J Dermatol. 2012;167(3):668-677.
14. Mamolo C, Harness J, Tan H, Menter A. Tofacitinib (CP-690,550), an oral Janus kinase inhibitor, improves patient-reported outcomes in a phase 2b, randomized, double-blind, placebo-controlled study in patients with moderate-to-severe psoriasis. J Eur Acad Dermatol Venereol. Published online ahead of print January 7, 2013.
15. Papp KA, Langley RG, Sigurgeirsson B, et al. Efficacy and safety of secukinumab in the treatment of moderate-to-severe plaque psoriasis: a randomized, double-blind, placebo-controlled phase II dose-ranging study. Br J Dermatol. 2013;168(2):412-421.
16. McInnes IB, Kavanaugh A, Gottlieb AB, et al. Efficacy and safety of ustekinumab in patients with active psoriatic arthritis: 1 year results of the phase 3, multicentre, double-blind, placebo-controlled PSUMMIT 1 trial. Lancet, 2013;382(9894):780-789.
17. Strand V, Schett G, Stevens RM. Patient-reported Health-related Quality of Life with apremilast for psoriatic arthritis: a phase II, randomized, controlled study. J Rheumatol. 2013;40(7):1158-1165.
18. Verneuil L, Varna M, Ratajczak P, et al. Human skin carcinoma arising from kidney transplant-derived tumor cells. J Clin Invest. 2013;123(9):3797-801.
19. Schmults CD, Karia PS, Carter JB, Han J, Qureshi AA. Factors predictive of recurrence and death from cutaneous squamous cell carcinoma: a 10-year, single-institution cohort study. JAMA Dermatol. 2013;149(5):541-547.
20. Gamba CS, Clarke CA, Keegan TH, Tao L, Swetter SM. Melanoma survival disadvantage in young, non-Hispanic white males compared with females. JAMA Dermatol. 2013;149(8):912-920.
21. Hodi FS, Corless CL, Giobbie-Hurder A, et al. Imatinib for melanomas harboring mutationally activated or amplified KIT arising on mucosal, acral, and chronically sun-damaged skin. J Clin Oncol. 2013;31(26):3182-3190.
22. Wolchok JD, Kluger H, Callahan MK, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369(2):122-133.
23. American Association for Cancer Research. GM-CSF/Ipilimumab combination extends melanoma survival. Cancer Discov. 2013;3(7):OF6.
24. Castanedo-Tardana MP, Zug KA. Methylisothiazolinone. Dermatitis. 2013;24(1):2-6.
25. Malajian D, Belsito DV. Cutaneous delayed-type hypersensitivity in patients with atopic dermatitis. J Am Acad Dermatol. 2013;69(2):232-237.
26. Drolet BA, Frommelt PC, Chamlin SL, et al. Initiation and use of propranolol for infantile hemangioma: report of a consensus conference. Pediatrics. 2013;131(1):128-140.
27. Chan H, McKay C, Adams S, Wargon O. RCT of timolol maleate gel for superficial infantile hemangiomas in 5- to 24-week-olds. Pediatrics. 2013;131(6):e1739-e1747.
28. Saedi N, Metelitsa A, Patrell K, Arndt KA, Dover JS. Treatment of tattoos with a picosecond alexandrite laser: a prospective trial. Arch Dermatol. 2012;148(12):1360-1363.
29. FDA approves Botox Cosmetic to improve appearance of crow’s feet lines. FDA website. https://www.fda.gov/newsevents/newsroom/pressannouncements/ucm367662.htm. Accessed November 13, 2013.
30. Tangamornsuksan W, Chaiyakunapruk N, Somkrua R, Lohitnavy M, Tassaneeyakul W. Relationship between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson Syndrome and toxic epidermal necrolysis: a systematic review and meta-analysis. JAMA Dermatol. 2013;149(9):1025-1032.
The year 2013 has brought many exciting advances in the field of dermatology, particularly in the realm of biologic drugs and in melanoma treatment. In fact, there were so many discoveries that this year in review just touches on some of the highlights of the past year. Areas within the field of dermatology with recent significant advances include infectious disease, acne/rosacea, biologics, psoriasis, cutaneous malignancies, contact dermatitis, atopic dermatitis, pediatric dermatology, cosmetic dermatology and HLA allele associations.
Infectious Disease

MRSA Decolonization in Intensive Care Units
Huang et al found that washing every patient in intensive care units (ICUs) daily with chlorhexidine-impregnated cloths and 5 days of twice-daily intranasal mupirocin treatments reduced positive cultures of methicillin-resistant Staphylococcus aureus (MRSA) by 37% and reduced bloodstream infection from any pathogen by 44%.1 The study included 74,256 patients and 74 ICUs. Hospitals were divided into 3 groups: group 1, implemented MRSA screening and isolation; group 2, targeted decolonization (ie, screening, isolation and decolonization of MRSA carriers) and group 3, universal decolonization (ie, no screening and decolonization of all patients). Universal decolonization was more effective than targeted decolonization or screening and isolation in reducing rates of MRSA clinical isolates and bloodstream infection from any pathogen. This implies that our current standard of isolating patients with MRSA is less effective than previously believed.
New Antibiotics for the Treatment of Skin Infections
Tedizolid phosphate (Cubist Pharmaceuticals/Trius Therapeutics) may be a reasonable alternative to linezolid for treating acute bacterial skin and skin structure infections (ABSSSI), which includes cellulitis or erysipelas, major cutaneous abscesses and wound infections. ESTABLISH-1, a Phase III trial, found that 6-day oral tedizolid phosphate (200 mg once daily) was as effective as 10 days of oral linezolid (600 mg every 12 hours) for treatment of ABSSSI.2 Outcomes included early response, measured 48-72 hours after initiating therapy, and sustained clinical responses at the end of treatment (day 11) and at the post-therapy evaluation visit (7-14 days after the end of treatment); both early and sustained responses of tedizolid were non-inferior to linezolid. This shorter dosing period of tedizolid may also improve patient adherence.
The Medicines Company has developed oritavancin, a lipoglycopeptide with a long half-life and rapid bactericidal activity againstgram-positive bacteria, including MRSA. In fact, 1 single, 1200 mg intravenous (IV) dose of oritavancin was found to be as effective as a 7- to 10-day dose of vancomycin for acute bacterial and structural skin infections.3 At 48-72 hours there was cessation of spread or reduction in size of the baseline lesion, the absence of fever and no requirement for rescue antibiotics (82.3% for oritavancin vs 78.9% for vancomycin). MRSA infections had similar outcomes (80.8% for oritavancin vs 80.0% for vancomycin). Rates of adverse events were similar in the 2 groups; 60.0% of the oritavancin group reported at least 1 adverse event, as did 63.8% of the vancomycin group. If implemented, this antibiotic could substantially reduce hospital admissions for IV antibiotics.

New Topical Treatments for Tinea Pedis and Onychomycosis
The topical allylamine naftifine hydrochloride 2% gel (Merz North America) was found to be well-tolerated and effective in treating both interdigital-type and moccasin-type tinea pedis in a large, randomized, controlled trial.4 After only 2 weeks of daily application, patients treated with naftifine gel 2% demonstrated statistically significant improvement from baseline in terms of complete cure, mycological cure and treatment effectiveness. Improvements continued with time; at 6 weeks the treatment group achieved 22% complete cure, 62% mycologic cure and 52% treatment effectiveness (P< 0.0001 for all 3 categories). In July, Naftin (naftifine HCl) Gel 2%, (Merz North America) received FDA approval, for the treatment of interdigital tinea pedis caused by the organisms Trichophyton rubrum, T. mentagrophytes and Epidermophyton floccosum in patients 18 years of age and older.
Another topical antifungal agent, luliconazole cream 1% (Luzu, Topica Pharmaceuticals), an imidazole, was found in a double-blind, vehicle-controlled study to be safe and effective for treatment at 2 week or 4 weeks for interdigital tinea pedis.5 At 2 weeks, 26.8% of the treatment group achieved complete clearance, and at 4 weeks 45.7% achieved complete clearance (compared to controls 9.1% and 10.0%, respectively). More importantly, the antifungal effects of luliconazole persisted for several weeks, resulting in increased rates of mycological cure. Luliconazole cream 1% received FDA approval in November for the topical treatment of interdigital tinea pedis, tinea cruris and tinea corporis, caused by the organisms T. rubrum and E. floccosum, in patients 18 years of age and older.
Prior to this year, topical treatments for onychomycosis were only modestly effective. However, a novel topical triazole antifungal, efinaconazole (Valeant Pharmaceuticals International, Inc) was shown in Phase II and Phase III studies to be effective in treating mild-to-moderate toenail distal lateral subungual onychomycosis (DLSO).6,7 In Phase II studies, mycologic cure rates with efinaconazole 10% semiocclusion, efinaconazole 10% and efinaconazole 5% were 83%, 87% and 87%, respectively.6 At follow-up, complete cure was also higher in the treatment groups, ranging from 16%-26%. This study provided evidence that once-daily efinaconazole 10% solution applied topically for 36 weeks was more effective than vehicle in treating DLSO.
In these 2 Phase III studies, the treatment arm received 48 weeks of efinaconazole 10% solution, and were evaluated at week 52.7 Mycologic cure rates were significantly greater with efinaconazole, ranging from roughly 53%-55%. Complete cure in these studies ranged from 15%-18%. This is exciting news for patients and dermatologists alike, as the side-effect profile is much safer than oral medications.
Efficacy of Antimycobacterial Treatment in Sarcoidosis
The possibility for mycobacterial contribution in the pathogenesis of sarcoidosis prompted this Phase I, randomized, placebo-controlled trial of 30 patients with chronic cutaneous sarcoidosis.8 The trial investigated the role of concomitant levofloxacin, ethambutol, azithromycin and rifampin (CLEAR) therapy. Results showed the CLEAR group had statistically decreased lesion size and granuloma burden with 8 weeks of treatment compared to placebo. In the intention-to-treat analysis, the CLEAR-treated group experienced a decrease in mean index lesion size from 22.4 mm to 14.0 mm (P=0.008), whereas the 15 patients assigned to placebo experienced a non-significant increase in mean index lesion size from 17.1 mm to 17.9 mm (P=0.05 for the difference between groups).
Acne/Rosacea
New Treatment for Pre-Adolescent Acne
 On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
Brimonidine FDA Approved for Erythema Associated with Rosacea
On August 26, 2013, the FDA approved brimonidine topical gel 0.33% (Mirvaso, Galderma Laboratories) as the first and only topical treatment specifically indicated for the persistent facial erythema resulting from rosacea. It is a highly selective alpha-2 adrenergic receptor agonist and acts via vasoconstriction to improve erythema associated with rosacea. It is applied once daily to adults age 18 and older, and results last up to 12 hours.
 In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
Biologics
Omalizumab for Chronic Idiopathic or Spontaneous Urticaria
Genentech and Novartis Pharmaceuticals’ omalizumab (Xolair) was found to significantly reduce disease severity in patients with a chronic idiopathic urticaria who failed standard therapy. This Phase III, multi-center, randomized, double-blind study evaluated patients with moderate-to-severe chronic idiopathic urticaria who were still symptomatic while taking H-antihistamine therapy.11
After 12 weeks of treatment with omalizumab, the itch-severity score was significantly decreased in a dose-dependent relationship. Omalizumab, when administered as 3 doses of 150 mg or 300 mg at 4-week intervals, significantly reduced the weekly itch-severity score as compared with placebo; 150 mg of omalizumab (–8.1±6.4; P=0.001) and 300 mg of omalizumab (–9.8±6.0; P<0.001). Serious adverse events were rare, most of them occurring in the 300-mg group where they occurred in 6% of patients.
Adalimumab for Sarcoidosis
Adalimumab (Humira, AbbVie Inc) was effective in treating cutaneous sarcoidosis in a double-blind, randomized, placebo-controlled trial.12 After 12 weeks, there was improvement specifically in target lesion area in the adalimumab-treated patients relative to placebo recipients (P=.0203). At the end of the additional 12-week, open-label phase, there was significant improvement in target lesion area (P=.0063), target lesion volume (P=.0225) and Dermatology Life Quality Index score (P=.0034). While adalimumab was effective for cutaneous disease, it had no effect on pulmonary function tests, radiographic findings or laboratory studies.
Psoriasis
 Novel Janus Kinase Inhibitor Improves Psoriasis
Novel Janus Kinase Inhibitor Improves Psoriasis
Oral treatments are now being developed for psoriasis. Tofacitinib (Xeljanz, Pfizer Inc), a novel, oral Janus kinase inhibitor, has been shown to objectively and subjectively improve psoriasis. Results from Phase IIb trials found Psoriasis Area and Severity Index (PASI) 75 response rates were higher for all twice-daily doses: 25%, (2 mg), 41% (5 mg) and 67% (15 mg) compared to placebo (2%) at 12 weeks.13 Results from the Phase IIb, 12-week trial showed that tofacitinib also improved patient-reported outcomes.14 The study included patients with moderate-to-severe chronic plaque psoriasis who were candidates for systemic therapy or phototherapy. Treatment with tofacitinib 2 mg, 5 mg and 15 mg twice daily resulted in generally dose-dependent improvements in several patient-reported outcomes measures compared with placebo.
Secukinumab in Moderate-to-Severe Plaque Psoriasis
Novartis Pharmaceuticals’ secukin-umab, a fully human IgG1κ monoclonal anti-interleukin-17A antibody, was shown to significantly improve psoriasis in recent Phase II trials. After 12 weeks of treatment, 83% of patients randomized to receive 3 time monthly 150 mg doses achieved a PASI 75.15 In addition, 52% of the patients in this dosing regimen achieved a PASI 90 at 12 weeks. Secukinumab was well-tolerated, although 2 cases of neutropenia were reported in the treatment arm.
Ustekinumab for Psoriatic Arthritis
On September 23, 2013, ustekinumab (Stelara, Janssen Biotech Inc) alone or in combination with methotrexate was FDA approved for the treatment of psoriatic arthritis in patients age 18 and older. The fully human monoclonal antibody improved active psoriatic arthritis, despite treatment with disease-modifying anti-rheumatic drugs and/or non-steroidal anti-inflammatory drugs, in a Phase III trial (PSUMMIT 1).16 In the 45-mg group, 42.4% of patients saw a 20% improvement in their symptoms according to the criteria of the American College of Rheumatology (ACR20) at week 24. In the 90-mg group, 49.5% of patients achieved ACR20. In addition, ACR responses were greater with ustekinumab than placebo regardless of methotrexate use. Treatment was generally well-tolerated with similar proportions of patients in the treatment and placebo group experiencing adverse events at week 16.
Drug Therapy Improves Patient-Related Outcomes for Psoriatic Arthritis
A Phase IIb trial revealed that apremilast (Celgene Corporation), a specific inhibitor of phosphodiesterase 4, was successful at treating psoriatic arthritis as measured by several patient-related outcomes.17 Apremilast 20 mg twice a day resulted in statistically significant and clinically meaningful improvements in health-related quality of life, pain and global visual analog scale and Functional Assessment of Chronic Illness Therapy-Fatigue scores.
Cutaneous Malignancies

Donor Contribution to the Malignant Skin Epithelium in Kidney Transplantation
It is well-known that patients who receive organ transplants are at increased risk for squamous cell carcinoma. However, a new study found that it is possible that the actual donor may also contribute to this increased risk.18 In 21 skin squamous cell carcinomas from kidney transplant recipients, the researchers examined p53 expression TP53 mutations. In 1 patient, skin tumor cells that were the same genotype as the donated kidney also contained the same TP53 mutation. This may provide evidence for a donor contribution to the malignant skin epithelium in allogeneic kidney transplantation.
Risk Factors for Poor Outcome in Squamous Cell Carcinomas
In a new, single-center, 10-year retrospective, cohort study, 5 risk factors were identified that were associated with recurrence and death from cutaneous squamous cell carcinomas. The 5 major factors were: (1) tumor diameter of at least 2 cm; (2) invasion beyond fat; (3) poor cellular differentiation; (4) perineural invasion and (5) ear, temple or anogenital location.19 The researchers evaluated 985 patients who had a total of 1,832 tumors. The median follow-up was 50 months.
Melanoma Prognosis in Young Men
 A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
Imatinib for KIT-Mutatnt Melanomas
Imatinib (Gleevec, Novartis Pharmaceuticals) has shown efficacy in patients with KIT-mutant melanoma in a multi-center, Phase II trial.21 Of the patients with KIT mutations or amplification in melanomas arising from acral, mucosal or chronically sun-damaged sites, the response rate was 21%. KIT mutations should be analyzed in these locations, because imatinib now represents a viable treatment option.
Combination Therapy for Melanoma
In a Phase I trial, treatment of advanced melanoma with concurrent therapy of ipilimumab (Yervoy, Bristol-Myers Squibb) with the experimental nivolumab (Bristol-Myers Squibb) was very promising.22 The study examined both concurrent therapy and sequential therapy, and found the former to be superior. Furthermore, the objective response rates of concurrent therapy also exceeded the previously reported results of nivolumab and ipilimumab monotherapy. The superior response with combination therapy is thought to be secondary to targeting different immune checkpoints: ipilimumab is an antibody against cytotoxic T-lymphocyte-associated antigen 4, and nivolumab is an antibody against the programmed death 1 receptor. The objective response rate with the concurrent use of the 2 therapies was 40% (N=53 patients). Furthermore, in those patients receiving a maximum dose (associated with an acceptable level of adverse events), ipilimumab (3 mg/kg/day) and nivolumab (1 mg/kg/day), the objective response rate was 53%, all with tumor reduction of 80% or more. Adverse events were common with Grade 3 or Grade 4 therapy- related adverse events in 53% of patients in the concurrent regimen; however, these were manageable and were generally reversible. The most common side effects included elevated levels of lipase (13%), aspartate aminotransferase (13%) and alanine aminotransferase (11%).
A Phase II trial for metastatic melanoma also showed benefit with combination therapy; in this instance, ipilimumab was combined with a granulocyte-macrophage colony-stimulating factor, sargramostim (Leukine, sanofi-aventis).23 Combining therapy in this case not only prolonged survival, but caused fewer serious side effects and deaths compared with ipilimumab alone. The median overall survival for the combination was 17.5 months, while ipilimumab monotherapy was 12.7 months (P=.0014). There was also a 35% decrease in risk of dying with combination therapy than those treated with ipilimumab alone.
Contact Dermatitis
Methylisothiazolinone Is the Allergen of the Year
The American Contact Dermatitis Society named the preservative/biocide methylisothiazolinone (MI) as the 2013 Allergen of the Year.24 Methylisothiazolinone is found in face creams, mascaras, shampoos, body washes and wet wipes, and is increasingly being used in the United States. Patch testing with the methylchloroisothiazolinone/MI mix misses approximately 40% of those allergic to MI, most likely secondary to the low MI concentration in the mix. It is has been recommended that routine screening of MI take place with patch testing series.
Atopic Dermatology
Allergic Contact Dermatitis in Patients with Atopic Dermatitis
 Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Pediatric Dermatology
Recommendations for the Use of Propranolol in Infantile Hemangiomas
 Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Recommendations included when to treat complicated IH; contraindications and pre-treatment evaluation protocols; propranolol use in PHACE syndrome; formulation, target dose and frequency of propranolol; initiation of propranolol in infants; cardiovascular monitoring; ongoing monitoring and prevention of hypoglycemia. It was universally agreed that an electrocardiogram should be part of the pre-treatment evaluation in instances where patients had below normal heart rate, or if patients have a family history of arrhythmias or maternal history of connective tissue disease. The recommended initial dosing for propranolol was 1 mg/kg/day (at a concentration of 20 mg/5 mL) divided into 3 times daily and than titrated up to a target dose. It was also recommended that propranolol be discontinued during illness to prevent hypoglycemia. Furthermore, recommendations regarding ongoing monitoring and PHACE syndrome screening and treatment are outlined within the guidelines. These new guidelines are valuable to the medical community given the frequency that IH occur and the prior lack of recommendations.
Timolol for Hemangiomas
Timolol has been studied in non-randomized trials, but a recent randomized, controlled trial evaluated timolol maleate 0.5% gel on superficial focal hemangiomas in a 24-week study of infants age 5 to 24 weeks.27
The results showed timolol applied twice a day significantly reduced proportional growth and lesion volume compared to placebo. The efficacy of timolol was more pronounced for lesions with a mean diameter of <11.3 mm (<100 mm3). In addition, clinical appearance improved; the blinded photo evaluation at 24 weeks found that 47% of actively treated lesions were free of redness compared to only 6% of lesions in the placebo group. Patients treated with timolol gel began to show efficacy at 12 weeks to 16 weeks, much later than the effect seen after starting oral propranolol, which usually is noticeable at 48 hours. However, based on the study results, timolol appears safe with no significant differences in heart rate or systolic or diastolic blood pressures.
Cosmetic Dermatology
Picosecond 755-nm Alexandrite Laser for Tattoo Removal
 A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
OnabotulinumtoxinA FDA approved for Lateral Canthal Lines
 On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
HLA Allele Associations
HLA-B*1502 Allele Association with SJS and TEN in Patients Using Carbamazepine
A new meta-analysis showed a significant association between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) within specific races. Han-Chinese, Thais, Koreans and Malaysians have approximately 115-fold, 60-fold, 25-fold and 220-fold increased risk of developing SJS or TEN with this HLA allele, respectively.30 The FDA currently recommends HLA-B*1502 allele before initiation of carbamazepine therapy in Asian patients. Despite these recommendations, there was still some debate about the relationship between HLA-B*1502 and SJS and TEN among patients taking carbamazepine, especially within some races. These findings provide an overwhelming relationship between the HLA-B*1502 allele and carbamazepine-induced SJS and TEN within specific races, the implications of which will hopefully lead to more standardized genetic testing before initiation of carbamazepine therapy.
Summary
It has been another exciting year in dermatology. We appreciate all the dedicated clinicians and researchers that have contributed to this year’s dermatology advances, from oral medication for psoriasis to new treatment options for melanoma. We look forward to all scientific and therapeutic advances on the horizon for 2014 and beyond. n
Dr. De Luca is with the department of dermatology at Wake Forest University School of Medicine in Winston-Salem, NC.
Disclosure: Dr. De Luca has no conflicts of interest to report.
References
1. Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368(24):2255-2265.
2. Prokocimer P, De Anda C, Fang E, Mehra P, Das A. Tedizolid phosphate vs linezolid for treatment of acute bacterial skin and skin structure infections: the ESTABLISH-1 randomized trial. JAMA. 2013;309(6):559-569.
3. Corey R, Perez A, Moeck G, et al. A single-dose of oritavancin (ORI) is comparable to 7-10 days of vancomycin (VAN) in the treatment of acute bacterial skin and skin structure infections (ABSSSI): the SOLO I study. Presented at: 53rd Interscience Conference on Antimicrobial Agents and Chemotherapy; September 10, 2013; Denver, CO. Abstract L-204.
4. Stein Gold LF, Parish LC, Vlahovic T, et al. Efficacy and safety of naftifine HCl Gel 2% in the treatment of interdigital and Moccasin type tinea pedis: pooled results from two multicenter, randomized, double-blind, vehicle-controlled trials.
J Drugs Dermatol. 2013;12(8):911-918.
5. Jarratt M, Jones T, Kempers S, et al. Luliconazole for the treatment of interdigital tinea pedis: A double-blind, vehicle-controlled study. Cutis. 2013;91(4):203-210.
6. Tschen EH, Bucko AD, Oizumi N, Kawabata H, Olin JT, Pillai R. Efinaconazole solution in the treatment of toenail onychomycosis: a phase 2, multicenter, randomized, double-blind study.
J Drugs Dermatol. 2013;12(2):186-192.
7. Elewski BE, Rich P, Pollak R, et al. Efinaconazole 10% solution in the treatment of toenail onychomycosis: Two phase III multicenter, randomized, double-blind studies. J Am Acad Dermatol. 2013;68(4):600-608.
8. Drkae WF, Oswald-Richter K, Richmond BW, et al. Oral antimycobacterial therapy in chronic cutaneous sarcoidosis: a randomized, single-masked, placebo-controlled study. JAMA Dermatol. 2013;149(9):1040-1049.
9. Eichenfield LF, Draelos Z, Lucky AW, et al. Preadolescent moderate acne vulgaris: a randomized trial of the efficacy and safety of topical adapalene-benzoyl peroxides. J Drugs Dermatol. 2013;12(6):611-618.
10. Fowler J Jr, Jackson M, Moore A, et al. Efficacy and safety of once-daily topical brimonidine tartrate gel 0.5% for the treatment of moderate to severe facial erythema of rosacea: results of two randomized, double-blind, and vehicle-controlled pivotal studies. Drugs Dermatol. 2013;12(6):650-656.
11. Maurer M, Rosén K, Hsieh HJ, et al. Omalizumab for the treatment of chronic idiopathic or spontaneous urticaria. N Engl J Med. 2013;368(10):924-935.
12. Pariser RJ, Paul J, Hirano S, Torosky C, Smith M. A double-blind, randomized, placebo-controlled trial of adalimumab in the treatment of cutaneous sarcoidosis. J Am Acad Dermatol. 2013;68(5):765-773.
13. Papp KA, Menter A, Strober B, et al. Efficacy and safety of tofacitinib, an oral Janus kinase inhibitor, in the treatment of psoriasis: a Phase 2b randomized placebo-controlled dose-ranging study. Br J Dermatol. 2012;167(3):668-677.
14. Mamolo C, Harness J, Tan H, Menter A. Tofacitinib (CP-690,550), an oral Janus kinase inhibitor, improves patient-reported outcomes in a phase 2b, randomized, double-blind, placebo-controlled study in patients with moderate-to-severe psoriasis. J Eur Acad Dermatol Venereol. Published online ahead of print January 7, 2013.
15. Papp KA, Langley RG, Sigurgeirsson B, et al. Efficacy and safety of secukinumab in the treatment of moderate-to-severe plaque psoriasis: a randomized, double-blind, placebo-controlled phase II dose-ranging study. Br J Dermatol. 2013;168(2):412-421.
16. McInnes IB, Kavanaugh A, Gottlieb AB, et al. Efficacy and safety of ustekinumab in patients with active psoriatic arthritis: 1 year results of the phase 3, multicentre, double-blind, placebo-controlled PSUMMIT 1 trial. Lancet, 2013;382(9894):780-789.
17. Strand V, Schett G, Stevens RM. Patient-reported Health-related Quality of Life with apremilast for psoriatic arthritis: a phase II, randomized, controlled study. J Rheumatol. 2013;40(7):1158-1165.
18. Verneuil L, Varna M, Ratajczak P, et al. Human skin carcinoma arising from kidney transplant-derived tumor cells. J Clin Invest. 2013;123(9):3797-801.
19. Schmults CD, Karia PS, Carter JB, Han J, Qureshi AA. Factors predictive of recurrence and death from cutaneous squamous cell carcinoma: a 10-year, single-institution cohort study. JAMA Dermatol. 2013;149(5):541-547.
20. Gamba CS, Clarke CA, Keegan TH, Tao L, Swetter SM. Melanoma survival disadvantage in young, non-Hispanic white males compared with females. JAMA Dermatol. 2013;149(8):912-920.
21. Hodi FS, Corless CL, Giobbie-Hurder A, et al. Imatinib for melanomas harboring mutationally activated or amplified KIT arising on mucosal, acral, and chronically sun-damaged skin. J Clin Oncol. 2013;31(26):3182-3190.
22. Wolchok JD, Kluger H, Callahan MK, et al. Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med. 2013;369(2):122-133.
23. American Association for Cancer Research. GM-CSF/Ipilimumab combination extends melanoma survival. Cancer Discov. 2013;3(7):OF6.
24. Castanedo-Tardana MP, Zug KA. Methylisothiazolinone. Dermatitis. 2013;24(1):2-6.
25. Malajian D, Belsito DV. Cutaneous delayed-type hypersensitivity in patients with atopic dermatitis. J Am Acad Dermatol. 2013;69(2):232-237.
26. Drolet BA, Frommelt PC, Chamlin SL, et al. Initiation and use of propranolol for infantile hemangioma: report of a consensus conference. Pediatrics. 2013;131(1):128-140.
27. Chan H, McKay C, Adams S, Wargon O. RCT of timolol maleate gel for superficial infantile hemangiomas in 5- to 24-week-olds. Pediatrics. 2013;131(6):e1739-e1747.
28. Saedi N, Metelitsa A, Patrell K, Arndt KA, Dover JS. Treatment of tattoos with a picosecond alexandrite laser: a prospective trial. Arch Dermatol. 2012;148(12):1360-1363.
29. FDA approves Botox Cosmetic to improve appearance of crow’s feet lines. FDA website. https://www.fda.gov/newsevents/newsroom/pressannouncements/ucm367662.htm. Accessed November 13, 2013.
30. Tangamornsuksan W, Chaiyakunapruk N, Somkrua R, Lohitnavy M, Tassaneeyakul W. Relationship between the HLA-B*1502 allele and carbamazepine-induced Stevens-Johnson Syndrome and toxic epidermal necrolysis: a systematic review and meta-analysis. JAMA Dermatol. 2013;149(9):1025-1032.


 On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers. In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies. Novel Janus Kinase Inhibitor Improves Psoriasis
Novel Janus Kinase Inhibitor Improves Psoriasis 
 A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma. Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens. Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.  A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.  On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines. 







 On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers.
On February 19, 2013, the FDA approved adapalene and benzoyl peroxide gel 0.1%/2.5% (Epiduo, Galderma Laboratories) to treat acne in children as young as 9 years old. The multi-center, randomized, vehicle-controlled, double-blind, pediatric study evaluated the safety and efficacy of adapalene and benzoyl peroxide gel 0.1%/2.5% in 285 acne patients age 9 to 11.9 At the conclusion of the 12 weeks, 49.3% of the treatment group achieved overall treatment success, 68.6% had a reduction in total lesion counts, 63.2% had a reduction in inflammatory lesions and 70.7% had a reduction in non-inflammatory lesions (all with P<.001). This is the first FDA-approved drug for acne in this pre-adolescent age group. As the age of puberty increasingly occurs earlier in life, this medicine fills an increasing need for safe and effective acne treatment for younger patients, say researchers. In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies.
In the most recent Phase III clinical studies, brimonidine topical gel yielded significantly greater improvement in the facial redness of rosacea than vehicle gel, with a significant difference observed as early as 30 minutes after the first application on day 1.10 Brimonidine topical gel was safe and well-tolerated during the 4 weeks of application in both Phase III studies. No tachyphylaxis or rebound were observed. The most frequent related adverse events included worsening of erythema and/or flushing, pruritus, skin irritation and worsening of rosacea. Related adverse events in the 2 treatment groups ranged from 9.5%-11.6%, while the vehicle gel ranged from 5.3%-9.7%. The events, however, were mild and transient. There were no serious adverse events seen in these studies. Novel Janus Kinase Inhibitor Improves Psoriasis
Novel Janus Kinase Inhibitor Improves Psoriasis 
 A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma.
A study cohort of 26,107 non-Hispanic, white adolescents and young adults, age 15 to 39 years, with a primary invasive melanoma of the skin from the Surveillance, Epidemiology and End Results network of cancer registries for melanomas, found that young men were 55% more likely to die of melanoma than age-matched women.20 With a mean follow-up of 7.5 years, there were fewer melanoma cases in young males (39.8%) than females, but they accounted for 63.6% of the deaths from melanoma. This risk was irrespective of health insurance and socioeconomic status, suggesting a biologic difference in male and female melanoma. Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens.
Patients with atopic dermatitis were found to be significantly more likely to have positive patch testing than non-atopic patients (71.72% of atopic patients vs 64.49% of non-atopic controls had at least 1 positive patch test).25 This retrospective review compared the rates of positive patch test reactions to allergens on the North American Contact Dermatitis Group standard tray in 2,305 patients who were suspected of having allergic contact dermatitis. Along with finding that patients with atopic dermatitis were more likely to test positive, they were also found more likely to develop contact hypersensitivity to metal allergens including nickel sulfate, cobalt chloride and potassium dichromate. Prior literature on this relationship between atopic dermatitis and allergic contact dermatitis was mixed. This study suggests that atopic patients are at higher risk of developing cutaneous delayed hypersensitivity reactions and should be encouraged to avoid exposure to metal allergens. Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.
Pediatrics’ published guidelines this year for the treatment of infantile hemangiomas (IH).26 Recommendations came from a consensus conference, which first met on December 9, 2011. The expert panel was multi-institutional and multi-disciplinary. Until this report, there were no uniform guidelines for treatment.  A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.
A new picosecond 755-nm alexandrite laser (PicoSure, Cynosure) was found effective for the removal of tattoos, obtaining greater than 75% clearance in all 12 patients in the trial.28 In addition, all of the patients were satisfied or extremely satisfied with the treatment. The average number of treatment sessions needed to obtain 75% clearance was 4.25 treatments. Adverse effects included pain, swelling and blistering. In addition, dyspigmentation was reported at the 3-month follow-up.  On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.
On September 11, 2013, the FDA approved the use of onabotulinumtoxinA (Botox Cosmetic, Allergan) for temporary improvement in the appearance of moderate-to-severe lateral canthal lines in adults.29 It is currently the only FDA-approved drug treatment option for lateral canthal lines.