 Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
At the initial consultation patients are often taught about the pathophysiology of ACD: its delayed presentation; its relationship with the immune system (sensitization to a chemical and then elicitation of a dermatitis with re-exposure) and that it can occur at any point in time, even to something that the patient has been using regularly for a short period of time or intermittently for years. In certain cases, the topics of the other key players, such as irritant contact dermatitis (ICD) and contact urticaria, may be explained, as history (not patch testing) can point to these as the correct diagnosis for the patient. It is important to note that ICD, the most prevalent form of contact dermatitis, can at times precede or be a concomitant diagnosis with ACD.4,5 Unlike ACD, ICD occurs secondary to contact with an irritating or abrasive substance. Contact urticaria (wheal and flare reaction), on the other hand, represents the least prevalent form of ACD. It is an immune mediated phenomenon whose hallmark is an IgE and mast cell-mediated immediate-type hypersensitivity reaction. We acknowledge this form of hypersensitivity due to the severity of the potential deleterious anaphylactic type reactions and direct the reader to key sources.6-8
In this article, we discuss the 3 phases of patch testing and the critical role of nurses in patch testing.
Patch Testing
To itch or not to itch, that is the question so many patients struggle with. Do they put up with the discomfort of the pruritus, which can vary from mild to severe, or to relieve the discomfort only to have to deal with the side effects of steroids, antihistamines, creams etc? It can become a chronic, viscous cycle severely impacting their quality of life as well as a reduction in their overall health.
ACD is a very common disorder, yet it is not well understood by many health professionals. The irony is that almost everyone understands what causes poison ivy and how to avoid it. Nurses, especially those working with dermatologists who do patch testing, have a wonderful opportunity to play a critical role in helping these patients. The following is an outline of how the nurse can make a valuable difference in the diagnosis and patient outcome. Helping with a successful outcome is a truly a rewarding experience.
While there are multiple variables that can interfere with the ability to identify the source (or sources) of a patients’ dermatitis, there are also many opportunities to hone in on key information that can prove vital. At many of these steps, the nurse can be closely or even primarily responsible for acquiring vital data that can have a definite impact on a successful outcome. A successful outcome is defined as determining that the patient’s final diagnosis is a clinically relevant contact allergy confirmed by patch testing or the exclusion of such and the diagnosis of some other form of dermatitis. If the diagnosis is ACD, the percentage of patients experiencing a full or nearly full clearance can be very high. Even if the patch test does not lead to a definitive diagnosis of contact allergy, the testing could nevertheless be very helpful to both the clinician and the patient, allowing them to explore other causes of the dermatitis, provided the clinician is confident that all the correct steps during patch testing were followed.
Patch testing is divided into 3 phases of equal importance: pre-, interim- and post-testing.
Pre-Testing Phase
In the pre-testing phase, the nurse can provide valuable assistance by obtaining the patient’s response to the following questions:
• Where do you break out?
• If they respond with more than 1 location, is there any that is the most frequent and troublesome?
• How does a break out begin?
• Do you experience any pain, burning, itching, water blisters or feel like something is crawling on or in your skin?
• Is anyone else in your household experiencing problems?
• Is the problem more troublesome when you try to sleep?
• Are there any other sensations or problems you have noticed?
• As a child, did you have trouble with your skin? Or, did your mother tell you that? Do you have hay fever or asthma?
• Have you been given any kind of steroid for your rash, such as creams, pills or a shot in the muscle? If so, are they helpful?
• Is there anything you are suspicious of causing your problem?
Interim-Testing Phase
The next phase of testing is the preparation and application of the tests. If your physician uses the thin-layer rapid use epicutaneous (T.R.U.E.) Test (SmartPractice), the commercially available testing system that has a pre-set number of antigens prepared and ready to be applied, the nurse only needs to ensure that these have been stored at the proper temperature as listed and to check the expiration date. Because it is a peel and stick process, care must be taken that they are applied correct side up.
The use of individual antigens loaded into a chamber device, such as a Finn or IQ, presents the nurse with the sole responsibility in the most important part of the process. It is not merely loading the correct antigen into the corresponding chamber, but it is ensuring there is a uniform and adequate amount in each chamber. There must be enough antigen presented to the skin to ensure that allergic response can occur. Too little of the antigen can produce false-negatives, the biggest disservice to patients undergoing testing.
To maximize the utility of the test, proper placement is important. While the usual placement of the test is the upper back, all too often we are presented with upper backs that are not suitable for patch placement. Areas of recent sun exposure (sunburn or suntanned skin) have a decreased immune response and should be avoided for at least 3 weeks. Do not place patches over areas of active dermatitis. It is also important to assess the condition of the skin before application. If the skin is too dry, the patches will not adhere well. Skin that is too oily or moist is also problematic. Because the patient has been anticipating that the patches will be placed on their upper back, you must inform the patient why you need to look for other areas suitable to patching.
If the patches are placed in unsuitable areas, patch test reading/evaluation is extremely difficult. Uncertainty arises from the following questions. Are there false-negatives from decreased immune response? Are there false-positives from current dermatitis? Which antigen is reacting if there is widespread dermatitis? Thus, the patient has undergone an expensive, time-consuming test without any confidence in the validity of the results. However, with proper placement and consideration the nurse has contributed greatly to the validity of the test.
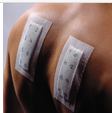
The goal post-application is to keep the patches in place, without shifting or lifting. This is a 2-fold goal. The first, no shifting, is to ensure the antigens are absorbed in the same location (ie, no intermingling of antigens and/or deposits of antigens in 2 or more areas). The second goal of no lifting is that when the patches are removed there is confidence that the antigens were absorbed by the skin. While there are a few physical measures to ensure the patches remain in place, such as additional taping, the instruction to keep the back completely dry and to keep movement to a minimum for the first 4 to 6 hours is the key.
Regardless of the system used, the adhesive will perform at its best if allowed to be warmed by the skin and undisturbed. Patients must be warned that care still needs to be taken for the remainder of the time that the patches are on, but the first 4 to 6 hours are extremely important. The nurse again has an important responsibility to help the patient assess what they will be doing in these critical hours and advise methods to ensure success.
Post-Patch Education Phase
The third phase, post-application/removal, is patient education. Nurses are often a vital component in this phase, as the patient may be overwhelmed or confused by the new information they have been given. If the diagnosis is ACD and they have shown sensitivity to 1 or more antigens, they will need to learn about products they can or cannot use.
There are several methods to guide patients on antigen avoidance, all of which are useful and produce a definite improvement in the patient’s dermatitis. Depending on the antigen, the number of antigens or the patient’s exposure (personal, occupational, hobby etc), the methodology for avoidance education varies. Primarily the 2 methods are instructions about where the antigens are primarily found and how to locate them (ie, on ingredient lists and material safety data sheets) or by providing the patients with a list of acceptable products (devoid of their identified allergens)based on the results of their patch testing. Appropriate barrier techniques must also be taught, especially in industrial or workplace exposures where avoidance of the antigen is not possible.
While the physician is responsible for determining the antigens to be placed and reading/interpreting the results, nurses can share the responsibility in helping to determine which antigens are appropriate by obtaining a meaningful history related to potential ACD, ensuring that the test itself, its proper placement and patient instructions provide the greatest potential for quality testing and ultimately, patient understanding of the results and appropriate actions to take. Nurses help patients help themselves post-patch testing by providing encouragement, understanding and support. n
Ms. Fowler is with Dermatology Specialists Research, LLC, in Louisville, KY.
References
1. Bickers DR, Lim HW, Margolis D, et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology and the Society for Investigative Dermatology. J Am Acad of Dermatol. 2006;55(3):490-500.
2. Hsu JW, Matiz C, Jacob SE. Nickel Allergy: localized, id, and systemic manifestations in children. Pediatr Dermatol. 2011;28(3):276-280.
3. Salam TN, Fowler JF Jr. Balsam-related systemic contact dermatitis. J Am Acad Dermatol. 2001;45(3):377-381.
4. Nijhawan RI, Matiz C, Jacob SE. Contact dermatitis: from basics to allergodromes. Pediatr Ann. 2009;38(2):99-108.
5. Militello G, Jacob SE, Crawford GH. Allergic contact dermatitis in children. Curr Opin Pediatr. 2006;18(4):385-390.
6. Valks R, Conde-Salazar L, Cuevas M. Allergic contact urticaria from natural rubber latex in healthcare and non-healthcare workers. Contact Dermatitis. 2004;50(4):222-224.
7. Walsh ML, Smith VH, King CM. Type 1 and type IV hypersensitivity to nickel. Australas J Dermatol. 2010;51(4):285-286.
8. Gimenez-Arnau A, Maurer M, De La Cuadra J, Maibach H. Immediate contact skin reactions, an update of Contact Urticaria, Contact Urticaria Syndrome and Protein Contact Dermatitis -- “A Never Ending Story.” Eur J Dermatol. 2010;20(5):552-562.
Dr. Jacob, the Section Editor of Allergen Focus, is associate clinical professor of medicine and pediatrics WOS (Dermatology) at the University of California, San Diego.
Disclosure: Dr. Jacob is an investigator for Smartchoice USA PREA-2 trial.
 Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
At the initial consultation patients are often taught about the pathophysiology of ACD: its delayed presentation; its relationship with the immune system (sensitization to a chemical and then elicitation of a dermatitis with re-exposure) and that it can occur at any point in time, even to something that the patient has been using regularly for a short period of time or intermittently for years. In certain cases, the topics of the other key players, such as irritant contact dermatitis (ICD) and contact urticaria, may be explained, as history (not patch testing) can point to these as the correct diagnosis for the patient. It is important to note that ICD, the most prevalent form of contact dermatitis, can at times precede or be a concomitant diagnosis with ACD.4,5 Unlike ACD, ICD occurs secondary to contact with an irritating or abrasive substance. Contact urticaria (wheal and flare reaction), on the other hand, represents the least prevalent form of ACD. It is an immune mediated phenomenon whose hallmark is an IgE and mast cell-mediated immediate-type hypersensitivity reaction. We acknowledge this form of hypersensitivity due to the severity of the potential deleterious anaphylactic type reactions and direct the reader to key sources.6-8
In this article, we discuss the 3 phases of patch testing and the critical role of nurses in patch testing.
Patch Testing
To itch or not to itch, that is the question so many patients struggle with. Do they put up with the discomfort of the pruritus, which can vary from mild to severe, or to relieve the discomfort only to have to deal with the side effects of steroids, antihistamines, creams etc? It can become a chronic, viscous cycle severely impacting their quality of life as well as a reduction in their overall health.
ACD is a very common disorder, yet it is not well understood by many health professionals. The irony is that almost everyone understands what causes poison ivy and how to avoid it. Nurses, especially those working with dermatologists who do patch testing, have a wonderful opportunity to play a critical role in helping these patients. The following is an outline of how the nurse can make a valuable difference in the diagnosis and patient outcome. Helping with a successful outcome is a truly a rewarding experience.
While there are multiple variables that can interfere with the ability to identify the source (or sources) of a patients’ dermatitis, there are also many opportunities to hone in on key information that can prove vital. At many of these steps, the nurse can be closely or even primarily responsible for acquiring vital data that can have a definite impact on a successful outcome. A successful outcome is defined as determining that the patient’s final diagnosis is a clinically relevant contact allergy confirmed by patch testing or the exclusion of such and the diagnosis of some other form of dermatitis. If the diagnosis is ACD, the percentage of patients experiencing a full or nearly full clearance can be very high. Even if the patch test does not lead to a definitive diagnosis of contact allergy, the testing could nevertheless be very helpful to both the clinician and the patient, allowing them to explore other causes of the dermatitis, provided the clinician is confident that all the correct steps during patch testing were followed.
Patch testing is divided into 3 phases of equal importance: pre-, interim- and post-testing.
Pre-Testing Phase
In the pre-testing phase, the nurse can provide valuable assistance by obtaining the patient’s response to the following questions:
• Where do you break out?
• If they respond with more than 1 location, is there any that is the most frequent and troublesome?
• How does a break out begin?
• Do you experience any pain, burning, itching, water blisters or feel like something is crawling on or in your skin?
• Is anyone else in your household experiencing problems?
• Is the problem more troublesome when you try to sleep?
• Are there any other sensations or problems you have noticed?
• As a child, did you have trouble with your skin? Or, did your mother tell you that? Do you have hay fever or asthma?
• Have you been given any kind of steroid for your rash, such as creams, pills or a shot in the muscle? If so, are they helpful?
• Is there anything you are suspicious of causing your problem?
Interim-Testing Phase
The next phase of testing is the preparation and application of the tests. If your physician uses the thin-layer rapid use epicutaneous (T.R.U.E.) Test (SmartPractice), the commercially available testing system that has a pre-set number of antigens prepared and ready to be applied, the nurse only needs to ensure that these have been stored at the proper temperature as listed and to check the expiration date. Because it is a peel and stick process, care must be taken that they are applied correct side up.
The use of individual antigens loaded into a chamber device, such as a Finn or IQ, presents the nurse with the sole responsibility in the most important part of the process. It is not merely loading the correct antigen into the corresponding chamber, but it is ensuring there is a uniform and adequate amount in each chamber. There must be enough antigen presented to the skin to ensure that allergic response can occur. Too little of the antigen can produce false-negatives, the biggest disservice to patients undergoing testing.
To maximize the utility of the test, proper placement is important. While the usual placement of the test is the upper back, all too often we are presented with upper backs that are not suitable for patch placement. Areas of recent sun exposure (sunburn or suntanned skin) have a decreased immune response and should be avoided for at least 3 weeks. Do not place patches over areas of active dermatitis. It is also important to assess the condition of the skin before application. If the skin is too dry, the patches will not adhere well. Skin that is too oily or moist is also problematic. Because the patient has been anticipating that the patches will be placed on their upper back, you must inform the patient why you need to look for other areas suitable to patching.
If the patches are placed in unsuitable areas, patch test reading/evaluation is extremely difficult. Uncertainty arises from the following questions. Are there false-negatives from decreased immune response? Are there false-positives from current dermatitis? Which antigen is reacting if there is widespread dermatitis? Thus, the patient has undergone an expensive, time-consuming test without any confidence in the validity of the results. However, with proper placement and consideration the nurse has contributed greatly to the validity of the test.
The goal post-application is to keep the patches in place, without shifting or lifting. This is a 2-fold goal. The first, no shifting, is to ensure the antigens are absorbed in the same location (ie, no intermingling of antigens and/or deposits of antigens in 2 or more areas). The second goal of no lifting is that when the patches are removed there is confidence that the antigens were absorbed by the skin. While there are a few physical measures to ensure the patches remain in place, such as additional taping, the instruction to keep the back completely dry and to keep movement to a minimum for the first 4 to 6 hours is the key.
Regardless of the system used, the adhesive will perform at its best if allowed to be warmed by the skin and undisturbed. Patients must be warned that care still needs to be taken for the remainder of the time that the patches are on, but the first 4 to 6 hours are extremely important. The nurse again has an important responsibility to help the patient assess what they will be doing in these critical hours and advise methods to ensure success.
Post-Patch Education Phase
The third phase, post-application/removal, is patient education. Nurses are often a vital component in this phase, as the patient may be overwhelmed or confused by the new information they have been given. If the diagnosis is ACD and they have shown sensitivity to 1 or more antigens, they will need to learn about products they can or cannot use.
There are several methods to guide patients on antigen avoidance, all of which are useful and produce a definite improvement in the patient’s dermatitis. Depending on the antigen, the number of antigens or the patient’s exposure (personal, occupational, hobby etc), the methodology for avoidance education varies. Primarily the 2 methods are instructions about where the antigens are primarily found and how to locate them (ie, on ingredient lists and material safety data sheets) or by providing the patients with a list of acceptable products (devoid of their identified allergens)based on the results of their patch testing. Appropriate barrier techniques must also be taught, especially in industrial or workplace exposures where avoidance of the antigen is not possible.
While the physician is responsible for determining the antigens to be placed and reading/interpreting the results, nurses can share the responsibility in helping to determine which antigens are appropriate by obtaining a meaningful history related to potential ACD, ensuring that the test itself, its proper placement and patient instructions provide the greatest potential for quality testing and ultimately, patient understanding of the results and appropriate actions to take. Nurses help patients help themselves post-patch testing by providing encouragement, understanding and support. n
Ms. Fowler is with Dermatology Specialists Research, LLC, in Louisville, KY.
References
1. Bickers DR, Lim HW, Margolis D, et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology and the Society for Investigative Dermatology. J Am Acad of Dermatol. 2006;55(3):490-500.
2. Hsu JW, Matiz C, Jacob SE. Nickel Allergy: localized, id, and systemic manifestations in children. Pediatr Dermatol. 2011;28(3):276-280.
3. Salam TN, Fowler JF Jr. Balsam-related systemic contact dermatitis. J Am Acad Dermatol. 2001;45(3):377-381.
4. Nijhawan RI, Matiz C, Jacob SE. Contact dermatitis: from basics to allergodromes. Pediatr Ann. 2009;38(2):99-108.
5. Militello G, Jacob SE, Crawford GH. Allergic contact dermatitis in children. Curr Opin Pediatr. 2006;18(4):385-390.
6. Valks R, Conde-Salazar L, Cuevas M. Allergic contact urticaria from natural rubber latex in healthcare and non-healthcare workers. Contact Dermatitis. 2004;50(4):222-224.
7. Walsh ML, Smith VH, King CM. Type 1 and type IV hypersensitivity to nickel. Australas J Dermatol. 2010;51(4):285-286.
8. Gimenez-Arnau A, Maurer M, De La Cuadra J, Maibach H. Immediate contact skin reactions, an update of Contact Urticaria, Contact Urticaria Syndrome and Protein Contact Dermatitis -- “A Never Ending Story.” Eur J Dermatol. 2010;20(5):552-562.
Dr. Jacob, the Section Editor of Allergen Focus, is associate clinical professor of medicine and pediatrics WOS (Dermatology) at the University of California, San Diego.
Disclosure: Dr. Jacob is an investigator for Smartchoice USA PREA-2 trial.
 Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
At the initial consultation patients are often taught about the pathophysiology of ACD: its delayed presentation; its relationship with the immune system (sensitization to a chemical and then elicitation of a dermatitis with re-exposure) and that it can occur at any point in time, even to something that the patient has been using regularly for a short period of time or intermittently for years. In certain cases, the topics of the other key players, such as irritant contact dermatitis (ICD) and contact urticaria, may be explained, as history (not patch testing) can point to these as the correct diagnosis for the patient. It is important to note that ICD, the most prevalent form of contact dermatitis, can at times precede or be a concomitant diagnosis with ACD.4,5 Unlike ACD, ICD occurs secondary to contact with an irritating or abrasive substance. Contact urticaria (wheal and flare reaction), on the other hand, represents the least prevalent form of ACD. It is an immune mediated phenomenon whose hallmark is an IgE and mast cell-mediated immediate-type hypersensitivity reaction. We acknowledge this form of hypersensitivity due to the severity of the potential deleterious anaphylactic type reactions and direct the reader to key sources.6-8
In this article, we discuss the 3 phases of patch testing and the critical role of nurses in patch testing.
Patch Testing
To itch or not to itch, that is the question so many patients struggle with. Do they put up with the discomfort of the pruritus, which can vary from mild to severe, or to relieve the discomfort only to have to deal with the side effects of steroids, antihistamines, creams etc? It can become a chronic, viscous cycle severely impacting their quality of life as well as a reduction in their overall health.
ACD is a very common disorder, yet it is not well understood by many health professionals. The irony is that almost everyone understands what causes poison ivy and how to avoid it. Nurses, especially those working with dermatologists who do patch testing, have a wonderful opportunity to play a critical role in helping these patients. The following is an outline of how the nurse can make a valuable difference in the diagnosis and patient outcome. Helping with a successful outcome is a truly a rewarding experience.
While there are multiple variables that can interfere with the ability to identify the source (or sources) of a patients’ dermatitis, there are also many opportunities to hone in on key information that can prove vital. At many of these steps, the nurse can be closely or even primarily responsible for acquiring vital data that can have a definite impact on a successful outcome. A successful outcome is defined as determining that the patient’s final diagnosis is a clinically relevant contact allergy confirmed by patch testing or the exclusion of such and the diagnosis of some other form of dermatitis. If the diagnosis is ACD, the percentage of patients experiencing a full or nearly full clearance can be very high. Even if the patch test does not lead to a definitive diagnosis of contact allergy, the testing could nevertheless be very helpful to both the clinician and the patient, allowing them to explore other causes of the dermatitis, provided the clinician is confident that all the correct steps during patch testing were followed.
Patch testing is divided into 3 phases of equal importance: pre-, interim- and post-testing.
Pre-Testing Phase
In the pre-testing phase, the nurse can provide valuable assistance by obtaining the patient’s response to the following questions:
• Where do you break out?
• If they respond with more than 1 location, is there any that is the most frequent and troublesome?
• How does a break out begin?
• Do you experience any pain, burning, itching, water blisters or feel like something is crawling on or in your skin?
• Is anyone else in your household experiencing problems?
• Is the problem more troublesome when you try to sleep?
• Are there any other sensations or problems you have noticed?
• As a child, did you have trouble with your skin? Or, did your mother tell you that? Do you have hay fever or asthma?
• Have you been given any kind of steroid for your rash, such as creams, pills or a shot in the muscle? If so, are they helpful?
• Is there anything you are suspicious of causing your problem?
Interim-Testing Phase
The next phase of testing is the preparation and application of the tests. If your physician uses the thin-layer rapid use epicutaneous (T.R.U.E.) Test (SmartPractice), the commercially available testing system that has a pre-set number of antigens prepared and ready to be applied, the nurse only needs to ensure that these have been stored at the proper temperature as listed and to check the expiration date. Because it is a peel and stick process, care must be taken that they are applied correct side up.
The use of individual antigens loaded into a chamber device, such as a Finn or IQ, presents the nurse with the sole responsibility in the most important part of the process. It is not merely loading the correct antigen into the corresponding chamber, but it is ensuring there is a uniform and adequate amount in each chamber. There must be enough antigen presented to the skin to ensure that allergic response can occur. Too little of the antigen can produce false-negatives, the biggest disservice to patients undergoing testing.
To maximize the utility of the test, proper placement is important. While the usual placement of the test is the upper back, all too often we are presented with upper backs that are not suitable for patch placement. Areas of recent sun exposure (sunburn or suntanned skin) have a decreased immune response and should be avoided for at least 3 weeks. Do not place patches over areas of active dermatitis. It is also important to assess the condition of the skin before application. If the skin is too dry, the patches will not adhere well. Skin that is too oily or moist is also problematic. Because the patient has been anticipating that the patches will be placed on their upper back, you must inform the patient why you need to look for other areas suitable to patching.
If the patches are placed in unsuitable areas, patch test reading/evaluation is extremely difficult. Uncertainty arises from the following questions. Are there false-negatives from decreased immune response? Are there false-positives from current dermatitis? Which antigen is reacting if there is widespread dermatitis? Thus, the patient has undergone an expensive, time-consuming test without any confidence in the validity of the results. However, with proper placement and consideration the nurse has contributed greatly to the validity of the test.
The goal post-application is to keep the patches in place, without shifting or lifting. This is a 2-fold goal. The first, no shifting, is to ensure the antigens are absorbed in the same location (ie, no intermingling of antigens and/or deposits of antigens in 2 or more areas). The second goal of no lifting is that when the patches are removed there is confidence that the antigens were absorbed by the skin. While there are a few physical measures to ensure the patches remain in place, such as additional taping, the instruction to keep the back completely dry and to keep movement to a minimum for the first 4 to 6 hours is the key.
Regardless of the system used, the adhesive will perform at its best if allowed to be warmed by the skin and undisturbed. Patients must be warned that care still needs to be taken for the remainder of the time that the patches are on, but the first 4 to 6 hours are extremely important. The nurse again has an important responsibility to help the patient assess what they will be doing in these critical hours and advise methods to ensure success.
Post-Patch Education Phase
The third phase, post-application/removal, is patient education. Nurses are often a vital component in this phase, as the patient may be overwhelmed or confused by the new information they have been given. If the diagnosis is ACD and they have shown sensitivity to 1 or more antigens, they will need to learn about products they can or cannot use.
There are several methods to guide patients on antigen avoidance, all of which are useful and produce a definite improvement in the patient’s dermatitis. Depending on the antigen, the number of antigens or the patient’s exposure (personal, occupational, hobby etc), the methodology for avoidance education varies. Primarily the 2 methods are instructions about where the antigens are primarily found and how to locate them (ie, on ingredient lists and material safety data sheets) or by providing the patients with a list of acceptable products (devoid of their identified allergens)based on the results of their patch testing. Appropriate barrier techniques must also be taught, especially in industrial or workplace exposures where avoidance of the antigen is not possible.
While the physician is responsible for determining the antigens to be placed and reading/interpreting the results, nurses can share the responsibility in helping to determine which antigens are appropriate by obtaining a meaningful history related to potential ACD, ensuring that the test itself, its proper placement and patient instructions provide the greatest potential for quality testing and ultimately, patient understanding of the results and appropriate actions to take. Nurses help patients help themselves post-patch testing by providing encouragement, understanding and support. n
Ms. Fowler is with Dermatology Specialists Research, LLC, in Louisville, KY.
References
1. Bickers DR, Lim HW, Margolis D, et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology and the Society for Investigative Dermatology. J Am Acad of Dermatol. 2006;55(3):490-500.
2. Hsu JW, Matiz C, Jacob SE. Nickel Allergy: localized, id, and systemic manifestations in children. Pediatr Dermatol. 2011;28(3):276-280.
3. Salam TN, Fowler JF Jr. Balsam-related systemic contact dermatitis. J Am Acad Dermatol. 2001;45(3):377-381.
4. Nijhawan RI, Matiz C, Jacob SE. Contact dermatitis: from basics to allergodromes. Pediatr Ann. 2009;38(2):99-108.
5. Militello G, Jacob SE, Crawford GH. Allergic contact dermatitis in children. Curr Opin Pediatr. 2006;18(4):385-390.
6. Valks R, Conde-Salazar L, Cuevas M. Allergic contact urticaria from natural rubber latex in healthcare and non-healthcare workers. Contact Dermatitis. 2004;50(4):222-224.
7. Walsh ML, Smith VH, King CM. Type 1 and type IV hypersensitivity to nickel. Australas J Dermatol. 2010;51(4):285-286.
8. Gimenez-Arnau A, Maurer M, De La Cuadra J, Maibach H. Immediate contact skin reactions, an update of Contact Urticaria, Contact Urticaria Syndrome and Protein Contact Dermatitis -- “A Never Ending Story.” Eur J Dermatol. 2010;20(5):552-562.
Dr. Jacob, the Section Editor of Allergen Focus, is associate clinical professor of medicine and pediatrics WOS (Dermatology) at the University of California, San Diego.
Disclosure: Dr. Jacob is an investigator for Smartchoice USA PREA-2 trial.
 Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.





 Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.
Allergic contact dermatitis (ACD) is a significant disease, which affects 14.5 million Americans each year.1 The economic impact of this disease is high in terms of both patient morbidity and loss of income, school and work, not to mention significant expenditures for visits to healthcare providers and for medicaments.1 Once patch testing is performed and a culprit has been identified, education becomes the critical intervention to ensure adherence to an avoidance regimen. With allergen avoidance, remission of the dermatitis ensues. If patients are unable to comply with the avoidance regimen, they become at risk for recurrent or sustained dermatitis or progression to a systematized presentation.2,3 In fact, education of the patient often begins before the diagnostic patch test is ever placed, to ensure that the patient has an appropriate understanding of potential outcomes, and their central role in both their disease and treatment.