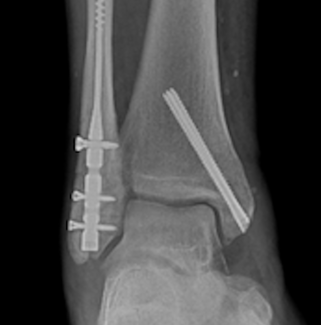
Total Ankle Replacement in Patients With Obesity: 10-Year Outcomes Challenge Traditional Contraindications
Long-term data on total ankle replacement (TAR) in patients with obesity have been limited and conflicting. This study provides over a decade of follow-up, offering important insights into functional outcomes, complication rates, and the role of obesity in surgical decision-making.
Key Takeaways
-
This study found that obesity does not negatively impact long-term TAR outcomes, with equivalent improvements in pain, function, and quality of life at ≥10 years.
-
The researchers saw similar secondary procedure and revision rates between obese and nonobese cohorts.
-
The data suggests that BMI alone should not be considered a contraindication to total ankle replacement in appropriately selected patients.
Total ankle replacement (TAR) has historically been approached with caution in patients with obesity due to concerns about complications and implant failure. However, this large retrospective cohort study evaluated 515 TAR procedures with a mean follow-up of 13.2 years, including over 300 cases with minimum 10-year patient-reported outcomes (PROMs), to better define long-term outcomes.1
Patients were stratified by body mass index (BMI ≥30 vs <30), and outcomes were assessed using validated tools including the Ankle Osteoarthritis Scale (AOS) and SF-36. The study represents one of the longest follow-ups to date examining obesity as a risk factor in TAR.1
Comparable Functional Outcomes Regardless of BMI
Both obese and nonobese cohorts experienced significant and sustained improvements in pain, function, and overall health status following TAR. Importantly, there were no statistically significant differences in improvement between groups for AOS pain/disability or SF-36 physical and mental scores over time.1
Although patients with obesity had worse baseline disability scores preoperatively, postoperative outcomes were comparable. Multivariable regression analysis confirmed that obesity (BMI ≥30) was not independently associated with worse long-term outcomes after adjusting for confounders such as age, diabetes, and implant type.1
Additionally, similar proportions of patients in both groups achieved clinically meaningful improvements, reinforcing that obese patients derive equivalent benefit from TAR.
Secondary Procedures and Revision Risk
Concerns about higher complication or revision rates in patients with obesity were not supported by the findings. Rates of secondary procedures were similar between cohorts (34.4% in obese vs 37.6% in nonobese), with no difference in major (“significant indication”) reoperations such as infection or implant failure.
The data further demonstrates comparable distributions of reoperation types, including revisions, debridement, and hardware-related procedures, across BMI groups. Time to secondary intervention was also similar, suggesting no accelerated failure pattern in patients with obesity.1
Clinical Implications: Reconsidering Obesity as a Contraindication
These findings challenge the longstanding perception of obesity as a relative contraindication to TAR. Despite biomechanical concerns, these patients experienced durable improvements over more than a decade, without increased procedural burden or worse outcomes.
The authors suggest that appropriate patient selection—rather than BMI alone—should guide surgical decision-making. This aligns with broader trends toward individualized risk assessment in musculoskeletal surgery.
Reference
1. Haider Z, Pinsker E, Fayyaz K, Khan R, Daniels T, Halai M. Total ankle replacement outcomes in obese patients with minimum 10-year follow-up. JBJS Open Access. 2026;11:e26.00054. doi:10.2106/JBJS.OA.26.00054
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.