Utilizing Multidisciplinary Care for a Patient With Dermatillomania
Key Clinical Takeaways
- Dermatillomania (US, SAWC Spring 2026): Skin picking disorder can cause tissue damage, infection, and severe complications; underlying lesions may be obscured by skin damage.
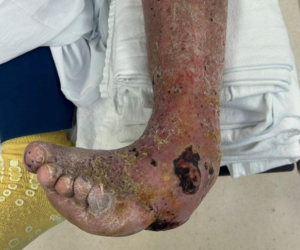
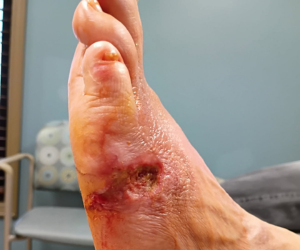
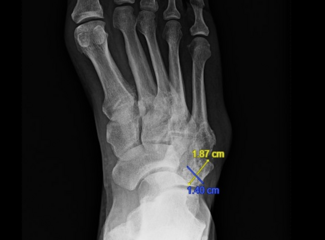
- Case (n=1): 64-year-old female with diabetes, anxiety, depression developed deep foot wounds and osteomyelitis, requiring hallux and third toe amputation; poor adherence initially.
- Clinical management: Multidisciplinary care (psychiatry + wound care) improved adherence and led to complete healing post-amputation; treatment includes behavioral therapy, medication, local wound care, and infection education.
Multidisciplinary care, particularly from mental health professionals, is crucial for patients with dermatillomania to mitigate the serious complications of the disorder, according to a case study poster presented at the Symposium on Advanced Wound Care (SAWC) Spring.
Dermatillomania, also known as skin picking disorder, can lead to tissue damage, infection, and potentially more serious health consequences, notes the poster.1 The authors note it can be difficult to determine the underlying cause because the overlying skin damage may mask the underlying primary lesion.
The case study involved a 64-year-old female who patient presented with skin injury to her hallux and third toe.1 Her history included poorly controlled diabetes, anxiety, depression, and prior psychiatric evaluations. The patient received treatment for her wound and psychiatric conditions but did not adhere well to treatment and developed deep wounds to her right foot toes as well as osteomyelitis. She ultimately underwent amputations of the right hallux and third toe.
The authors note psychiatry was consulted to manage the dermatillomania disorder and the patient’s treatment regimen was targeted with a multidisciplinary approach.1 Wound care and close outpatient follow-up continued. The poster notes the patient was able to adhere to the treatment and achieved complete healing of the surgical sites without complications.
Poster author Patrick McEneaney, DPM, notes multidisciplinary care is essential in managing dermatillomania because podiatrists, primary care physicians, or dermatologists are often the ones to identify skin picking. The lesions or wounds need local care handled by dermatologists, podiatrists or wound care professionals and he notes providers must maintain a high index of suspicion for this condition.
Dermatillomania is classified as an obsessive-compulsive and related disorder, so it is associated with comorbidities like depression and anxiety, emphasizes Dr. McEneaney. As he notes, long-term resolution is unlikely unless a psychiatrist and/or psychologist addresses the underlying behavioral and psychological components. He says behavioral therapy and medication are mainstays for treatment.
“Podiatrists need to build a relationship with their patients so that the patient is comfortable sharing their experiences,” says Dr. McEneaney. “These behaviors carry a stigma and cause shame for the patients which they don’t always like to share with anyone, including their doctor.”
Building trust happen through listening to the patient and once this trust is present, Dr. McEneaney says the podiatrist can explain the importance of referral to a mental health specialist. Dr. McEneaney also notes podiatrists can provide local wound care for open wounds and topical steroid creams for irritated areas. He stresses the importance of educating patients on the signs and symptoms of infection that can occur.
Reference
1. McEneaney P, Kolyesnykov P, Lovato P, Statkus R. An unusual complication of dermatillomania: amputation of two toes. Poster presented at the Symposium on Advanced Wound Care (SAWC) Spring, Charlotte, NC, April 8–12, 2026.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.