Left Atrial Appendage Occlusion Outside the Box: New Frontiers in Patient Selection
Key Summary
- Left atrial appendage occlusion (LAAO) is moving beyond traditional use in patients with nonvalvular AF patients who are unable to take anticoagulation, with emerging data supporting broader, individualized patient selection.
- Three-year results from the CHAMPION trial showed the WATCHMAN FLX was noninferior to NACs for stroke/CV death/systemic embolism and significantly reduced nonprocedural bleeding in anticoagulation-eligible patients.
- Concomitant procedures (eg, AF ablation, TAVR) and alternative strategies for no-antithrombotic patients are reshaping LAAO’s role in stroke prevention.
Rethinking Indications for Left Atrial Appendage Occlusion
Current US indications for left atrial appendage occlusion (LAAO) focus on patients with nonvalvular atrial fibrillation (AF) who are at increased stroke risk yet unsuitable for long-term anticoagulation. This presentation from Saibal Kar, MD, FSCAI, at the 2026 Society for Cardiovascular Angiography & Interventions (SCAI) Scientific Sessions, challenged that binary framework—patients who can or cannot tolerate long-term anticoagulation—and explored emerging evidence supporting broader, more nuanced patient selection.
LAAO vs NOACs in Anticoagulation-Eligible Patients
CHAMPION trial—for which Dr Kar serves as co-principal investigator —which sought to determine if Boston Scientific’s WATCHMAN device was noninferior to non-vitamin K antagonist oral anticoagulants (NOACs) in this population.
The largest randomized comparison (~3000 patients) of LAAO using the WATCHMAN FLX vs NOACs in patients eligible for anticoagulation, CHAMPION had 3 primary endpoints based on efficacy and safety. The first 2 endpoints were evaluated at 3 years: (1) noninferiority for a composite of ischemic and hemorrhagic stroke, cardiovascular death, and systematic embolism; and (2) superiority for non-procedural bleeding. The third endpoint of noninferiority for all thromboembolic events will be determined at 5 years.
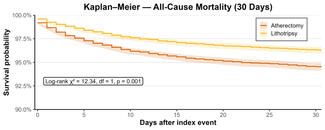
While results favored NOACs for the first 3-year endpoint, LAAO succeeded in demonstrating noninferiority (4.8% vs 5.7%; P < .001), even though ischemic events were slightly higher in the device arm. For the second primary endpoint, the results showed significant reduction in clinically relevant nonprocedural bleeding with LAAO vs NOACs (10.9% vs 19%; P < .001).
Following his presentation at the 2026 American College of Cardiology meeting in March, Dr Kar said of CHAMPION, “data suggest that the LAA closure device used in this trial is a potential and reasonable alternative to medication, even among patients who are suitable for long-term blood thinners, and may be discussed as part of a shared decision-making process.”1
Findings from the longer-term outcomes remain critical for informing the standard of care for these patients.
Managing Patients Who Cannot Take Any Antithrombotic Therapy
At the opposite extreme are patients who cannot tolerate even short-term anticoagulation or antiplatelet therapy, a group not currently indicated for WATCHMAN.
Alternative strategies include:
- Surgical LAA closure (ligation, excision, stapling)
- Percutaneous transpericardial ligation (eg, the LARIAT procedure)
- Endovascular devices
A benefit of the first 2 strategies is that they do not involve an implant in the left atrium, which in turn leads to a lower probability of device-related thrombus. The no-implant techniques are effective at closing the LAA, and endovascular occlusion is supported by real-world (albeit single-arm) registry data in both safety and efficacy.
The ASAP-TOO trial was designed to evaluate WATCHMAN with short-term dual antiplatelet therapy vs no therapy in this patient population; however, it was under-enrolled with just over half of the planned subjects. The results were presented at the 2026 Heart Rhythm Society (HRS) Scientific Sessions.
Concomitant Procedures: A Rising Trend
Combining LAAO with other interventions is rapidly expanding, with 25% of WATCHMAN implants currently performed alongside AF ablation in the United States; this number is expected to rise, thanks in part to the 2024 Medicare payment classification (MS-DRG 317) that covers these procedures so long as they are performed concomitantly.
While ablation is the most common concomitant procedure by far (73.2%, according to 2016-2020 numbers from the National Inpatient Sample database), the combination of TAVR, PPM implantation, ASD/PFO closure, PCI, TEER, and TMVR with LAAO have all been reported.
The OPTION trial was designed to see if LAAO (WATCHMAN FLX) following catheter ablation was a “reasonable alternative” to OACs for patients with NVAF. What it found was that there was no difference in stroke, all-cause death, or systemic embolism at 3 years when LAAO was combined with ablation, but also that there was a significant reduction in bleeding in the LAAO group, thereby supporting the concomitant performance of LAAO and ablation.
While not featured in any trial in the presentation, Dr Kar maintained that the most important concomitant procedure is, in fact, MV repair, emphasizing its procedural efficiency and potential clinical benefit. Mitral interventions are particularly attractive given shared transseptal access and no added contrast burden; plus, surgical guidelines already recommend LAAO during MV surgery.
According to Dr Kar, “the future should be TEER followed by LAAC followed possibly by [pulsed field ablation].”
Valvular Disease and Hybrid Approaches
Use of LAAO in valvular AF, especially rheumatic mitral stenosis, remains controversial due to concerns about increased risk of stroke and device-related thrombus. However, hybrid strategies may offer solutions in select high-risk patients who cannot tolerate anticoagulation. Case in point: an 82-year-old woman with rheumatic mitral stenosis, permanent AFib, and history of gastrointestinal bleeding who could not take any anticoagulation. She underwent a balloon mitral commissurotomy followed by transpericardial LAA ligation and has since, reports Dr Kar, done “very well.”
Implications and Conclusions
- LAAO is moving beyond traditional contraindication-based use
- Evidence supports consideration in both extremes: patients who can and cannot take anticoagulation
- Concomitant procedures represent a major growth area with favorable safety and economic implications
As evidence evolves, LAAO is poised to become a more versatile tool in stroke prevention across a broader AF population.
Dr Kar is an interventional Cardiologist at Los Robles Regional Medical Center, Thousand Oaks, California.
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of the Journal of Invasive Cardiology or HMP Global, their employees, and affiliates.